
The post How GLP-1 Agonists Can Help Support Perimenopause Symptoms appeared first on HUM Nutrition Blog.
]]>How GLP-1 Agonists Help with Perimenopause

GLP-1 (glucagon-like peptide-1) agonists work by mimicking the natural GLP-1 hormone in our body, which regulates blood sugar, appetite, and metabolism. These medications, such as semaglutide (Ozempic, Wegovy), tirzepatide (Mounjaro, Zepbound), and liraglutide (Saxenda, Victoza), have shown promising effects in managing some of the most frustrating aspects of perimenopause.
Insulin Sensitivity
As estrogen levels fluctuate during perimenopause, many women become more insulin resistant, increasing the risk of type 2 diabetes and metabolic disorders. This resistance can lead to energy crashes, sugar cravings, and difficulty maintaining stable blood sugar levels. Insulin resistance can also contribute to stubborn weight gain, particularly around the abdomen, making it even more challenging to maintain a healthy body composition.
However, GLP-1 medications like Wegovy and Ozempic help the body use insulin more effectively by increasing insulin sensitivity after eating and slowing glucose production in the liver. By improving how the body processes sugar, these medications can help prevent the metabolic disruptions that often come with perimenopause. Improving insulin regulation not only reduces blood sugar spikes and crashes but also minimizes sugar cravings and fatigue. Over time, control over insulin sensitivity can lower the risk of developing type 2 diabetes and support overall metabolic health during perimenopause.
Weight Management
One of the biggest challenges that women face during perimenopause is weight gain, especially around the abdomen area. Hormonal fluctuations can slow the metabolism, increasing fat storage and making it more difficult to maintain a healthy weight. Lower estrogen levels also play a role in where fat is distributed, leading to more weight gain around the midsection as opposed to other areas. This affects body composition and increases the risk of metabolic disorders, such as insulin resistance and cardiovascular disease.
GLP-1 medications can help with weight loss by promoting feelings of fullness and reducing appetite, leading to an overall decrease in one’s calorie intake. It also slows gastric emptying, keeping you satisfied for longer periods. As a result, appetite control combined with improved metabolic function helps support weight management, reducing perimenopausal weight gain.
These medications also help curb the cycle of sugar cravings and energy crashes that can often lead to overeating. Altogether, women find that using GLP-1’s alongside a balanced diet and regular exercise makes it easier to maintain a healthy weight during perimenopause, reducing the physical and emotional strain that weight fluctuations can bring.
Hot Flashes
Hot flashes are one of the most well-known—and often most bothersome—symptoms of perimenopause, occurring in 75% of women. These sudden surges of heat, sweating, and discomfort are the result of fluctuations in estrogen levels, affecting the body’s temperature regulation system. They’re known to disrupt sleep, impact daily activities, and leave many searching for relief.
While research is still developing, some studies suggest that GLP-1 medications may play a role in reducing the frequency and severity of hot flashes. GLP-1’s effects on the central nervous system and metabolic regulation may contribute to temperature stability. GLP-1 agonists help regulate neurotransmitters involved in thermoregulation, balancing the body’s temperature and resulting in fewer (and less intense) hot flashes during perimenopause. Additionally, since blood sugar fluctuations can sometimes exacerbate hot flashes, the improved glucose control offered by GLP-1 medications may indirectly reduce the severity.
Hormonal Balance
Perimenopause is caused by fluctuating hormone levels, leading to symptoms like mood swings, brain fog, fatigue, and irregular menstrual cycles. Although GLP-1 medications are not a direct hormonal therapy, they can indirectly support hormonal balance by improving insulin regulation and reducing inflammation—both of which can impact overall hormone health.
Inflammation is known to play a role in hormonal imbalances, and GLP-1s have been shown to reduce systemic inflammation, which may help alleviate symptoms like mood swings and metabolic issues commonly experienced. Additionally, by supporting metabolic health and weight management, GLP-1s may help reduce the severity of perimenopausal symptoms related to hormonal imbalances, such as fatigue and brain fog. Maintaining stability in blood sugar levels may also contribute to fewer extreme mood fluctuations, making the emotional symptoms of perimenopause more manageable.
FAQ’s
Are GLP-1s safe to use for perimenopause?
While these medications are FDA-approved for diabetes and weight loss, their use for perimenopause is considered off-label. Always consult a healthcare provider to see if this option is appropriate based on your individual health needs.
How long does it take to see results with GLP-1s during perimenopause?
Results can vary. Some women notice reduced appetite and better energy levels within the first few weeks, while improvements in weight and mood may take a few months. It’s a gradual process that works best when combined with lifestyle changes like diet, exercise, and stress management.
Can I use GLP-1 medications during menopause too?
Yes. Many women continue to experience symptoms well into menopause, and the benefits of GLP-1s—like weight control and improved blood sugar regulation—can still be valuable during that time.
Perimenopause is a complex phase of life, but GLP-1 medications have been shown to offer positive support for some of its most uncomfortable symptoms. From aiding in weight management and improving insulin sensitivity to potentially easing hot flashes and promoting hormonal balance, these medications may be valuable for women seeking relief. As research continues, GLP-1s are working to become a more widely recognized option for managing perimenopause effectively. If you’re considering this approach, consulting a healthcare provider can help determine if GLP-1 therapy is right for you.
The post How GLP-1 Agonists Can Help Support Perimenopause Symptoms appeared first on HUM Nutrition Blog.
]]>The post How to Balance Hormones: An Easy Guide to What They Are and What They Do, Including GLP-1 and Insulin appeared first on HUM Nutrition Blog.
]]>
Hormones are the body’s tiny chemical messengers that quietly influence everything from your sleep and stress to your cravings, weight, and even your skin. Most of the time, you don’t even notice they’re there—until they’re trying to get your attention. That’s when understanding your hormones becomes a game-changer.
Whether you’re looking to understand why you feel off some days, or you’re curious how to better support your body, getting a handle on your hormones is a smart move. And the good news? With the right knowledge (and a little help from science-backed supplements), you can help support hormonal balance naturally.
Let’s get into what hormones do, how they affect your body, and the key players you should know.
What Are Hormones and What Do They Do for the Body?
Hormones are chemicals produced by glands in the endocrine system, and they’re released into the bloodstream. They act as messengers, traveling through your body to tissues and organs, regulating growth, metabolism, mood, reproduction, and more. Hormones are essential for maintaining homeostasis, or a balanced internal environment in the body, and they influence how our organs and tissues function. Hormones help regulate a wide range of essential functions, including:
- Metabolism (how your body uses energy)
- Mood and emotions
- Sleep and wake cycles
- Growth and development
- Reproduction and sexual health
- Hunger and fullness
- Stress response
Even small shifts in hormone levels can have noticeable effects, which is why keeping them in balance is so crucial for your overall health and well-being.
Here are some of the most important hormones and what they do in the body.
Hormones Explained and How to Balance Them
GLP-1
Glucagon-like peptide-1 (GLP-1) is a hormone naturally produced in the gut. It plays a major role in regulating glucose metabolism and appetite. When we eat, GLP-1 is released into the bloodstream, signaling the pancreas to release insulin, which helps lower blood sugar levels. GLP-1 also reduces hunger by signaling to the brain that we’re full, playing a major role in regulating our eating behaviors. Additionally, it slows down gastric emptying, which helps you feel satisfied for longer periods after eating. Due to its ability to regulate glucose levels and appetite, it’s widely used as a supplement to promote weight loss.
How HUM Supplements Provide Support: HUM’s Flatter Me Fiber GLP-1 Booster benefits GLP-1 levels by promoting its release supporting healthy digestion and promoting feelings of fullness. The supplement includes ingredients designed to boost fiber intake, which can help regulate gastric emptying and improve satiety, similar to how GLP-1 functions. By promoting these processes, Flatter Me may help further enhance appetite control and support healthier glucose metabolism, aligning with the natural role of GLP-1 in regulating hunger and blood sugar.
Estrogen
Estrogen is one of the primary sex hormones in females. The hormone regulates the menstrual cycle, supports reproductive health, and maintains bone density. During puberty, it triggers the development of secondary sexual characteristics like breast development and the widening of hips. Estrogen also affects mood, skin health, and cardiovascular function. As women approach menopause, estrogen levels decrease, which can contribute to symptoms like hot flashes, mood changes, and an increased risk of osteoporosis.
How HUM Supplements Provide Support: HUM’s Hormone Balance supplement can help balance estrogen levels and overall hormonal health. Hormone Balance also contains ingredients like Chaste Berry and Dong Quai, which are known to support healthy estrogen levels, alleviate symptoms of PMS, and help regulate hormonal fluctuations, especially during times like menopause, when estrogen levels drop.
Progesterone
Progesterone is another key hormone in the female reproductive system. It helps regulate the menstrual cycle by preparing the uterus for a possible pregnancy after ovulation. If pregnancy doesn’t occur, progesterone levels drop, which signals the start of a new menstrual cycle. If pregnancy does happen, progesterone continues to support the uterine lining and helps maintain a healthy pregnancy in the early stages. Beyond reproduction, progesterone has a calming effect on the body, promoting better sleep and emotional balance. It also works alongside estrogen to maintain hormonal balance—while estrogen stimulates tissue growth, progesterone helps moderate it. In short, progesterone is key not only for reproductive health but also for mood regulation and overall hormonal harmony.
How HUM Supplements Provide Support: Private Party promotes a healthy vaginal environment, which can indirectly support reproductive health. Hormone Balance also includes ingredients that help regulate hormone fluctuations, like those associated with progesterone, supporting menstrual cycle regularity and alleviating PMS symptoms. Both supplements work in tandem to help maintain hormonal equilibrium, improving mood, and overall reproductive health.
Leptin and Ghrelin
Leptin and ghrelin are hormones that regulate hunger and satiety, working in tandem to control appetite.
- Leptin is a hormone produced by fat cells and plays a key role in regulating hunger and energy balance. It acts as a messenger to the brain, letting it know when your body has enough stored energy (fat) and doesn’t need more food. When leptin levels are high, it signals that you’re full and can stop eating. On the other hand, when leptin levels are low, your brain gets the message that you’re running low on energy, which increases your appetite. This system is meant to help maintain a healthy weight and prevent overeating.
- Ghrelin, often referred to as the “hunger hormone,” is produced mainly in the stomach and is responsible for stimulating appetite. When your stomach is empty, ghrelin levels rise, sending a message to your brain that you’re hungry. This hormone not only encourages you to eat but also plays a role in meal initiation and food-seeking behavior. Once you’ve eaten, ghrelin levels decrease, contributing to the feeling of fullness and satisfaction after a meal. Ghrelin levels tend to rise before meals and fall afterward in a natural rhythm. Sleep deprivation, stress, and restrictive dieting can disrupt this pattern, leading to higher ghrelin levels and increased hunger—making it harder to stick to healthy eating habits.
Together, these hormones work to maintain a balanced energy intake and prevent overeating or under-eating.
How HUM Supplements Provide Support: Flatter Me Fiber GLP-1 Booster can ease feelings of hunger by improving digestion and enhancing satiety. The fiber in this supplement helps slow gastric emptying, similar to the way GLP-1 functions, keeping you feeling full for longer periods. In general, fiber can help stabilize hunger hormones, helping reduce hunger signals.
Cortisol
Cortisol is often referred to as the “stress hormone” because the adrenal glands produce it in response to stress. When you encounter a stressful situation, cortisol is released to help your body deal with the stressor by going into “fight or flight” mode. It increases blood sugar levels, boosts energy, and has anti-inflammatory effects. While cortisol is necessary for dealing with short-term stress, chronic stress can lead to elevated cortisol levels, which may negatively affect the body by increasing the risk of weight gain, anxiety, depression, and other health issues.
How HUM Supplements Provide Support: Ashwagandha Calm Gummies help manage cortisol levels by reducing feelings of stress and promoting a sense of calm. Ashwagandha is an adaptogen known for its ability to help the body adapt to stress and balance cortisol production. Incorporating these gummies into your routine can help support the body in managing stress more effectively, potentially lowering chronic cortisol levels which can help minimize the adverse effects associated with long-term stress, like weight gain and anxiety.
Insulin
Insulin is a hormone produced by the pancreas that regulates blood sugar levels. When you eat, carbohydrates in food are broken down into glucose (sugar), which enters the bloodstream. Insulin helps cells absorb this glucose for energy or storage. Proper insulin function is critical for maintaining stable blood sugar levels. When the body becomes resistant to insulin (as in type 2 diabetes), glucose builds up in the bloodstream, leading to various health problems. Overtime, poor diet, lack of exercise, and genetics can all lead to insulin resistance.
How HUM Supplements Provide Support: Flatter Me Fiber GLP-1 Booster can support insulin function by helping to regulate glucose metabolism. The fiber content helps slow gastric emptying, promoting more stable blood sugar levels. Enhancing satiety and supporting healthy digestion may also help and support balanced blood sugar levels, contributing to better overall insulin sensitivity.
FAQ Section
Can hormone imbalances cause weight gain?
Yes, hormone imbalances can contribute to weight gain. For example, insulin resistance, cortisol imbalances, and thyroid hormone deficiencies are all linked to increased weight gain or difficulty losing weight.
How do hormones affect mood?
Hormones like estrogen, progesterone, and cortisol play a significant role in regulating mood. For instance, low estrogen levels can contribute to feelings of depression and anxiety, while high cortisol levels due to stress can lead to irritability or anxiety.
Can diet affect hormone levels?
Absolutely. Diet can influence hormone production and balance. For example, a diet high in processed foods and sugar can lead to insulin resistance, while nutrient-dense foods can support healthy hormone production.
How can I balance my hormones naturally?
Maintaining a healthy diet, regular exercise, good sleep hygiene, and managing stress are all essential for keeping hormones balanced. Taking science-backed supplements—like those from HUM Nutrition—can also support hormone health by filling in nutritional gaps and promoting overall balance in the body. However, in some cases, medical treatment may be necessary to address imbalances.
The Takeaway on How to Balance Hormones
Hormones are essential in our bodies, influencing everything from metabolism to mood and reproductive health. By understanding what these hormones do and how they affect us, we can make better lifestyle choices to keep them balanced. Whether eating a nutrient-rich diet, managing stress, or getting enough sleep, taking care of your hormonal health is key to maintaining overall well-being. If you suspect you’re dealing with a hormone imbalance, consulting a healthcare professional is a good first step in getting back on track.
The post How to Balance Hormones: An Easy Guide to What They Are and What They Do, Including GLP-1 and Insulin appeared first on HUM Nutrition Blog.
]]>The post Perimenopause Explained: The Best Supplements and How to Ease Symptoms appeared first on HUM Nutrition Blog.
]]>What is Perimenopause?

Perimenopause is the transitional phase before menopause when your body gradually reduces its production of estrogen and progesterone, the key hormones that regulate your menstrual cycle. Menstrual health practitioner Michelle Agudelo states that while it can vary from person to person, perimenopause typically occurs for women in their late 30s to early or mid-40s, lasting for four to eight years on average. During perimenopause, your periods may become irregular—sometimes heavier, sometimes lighter, or even skipping months altogether. While menopause officially begins when you’ve gone 12 consecutive months without a period, perimenopause can last for several years, bringing a variety of symptoms like mood swings, sleep disturbances, and hot flashes. The Journal of Obstetrics, Gynecology, and Cancer Research estimates that vasomotor symptoms (hot flashes) occur within 75-80% of perimenopausal women. Despite these numbers, understanding this phase can help you manage the changes and feel more in control of your health.
Causes
While the perimenopause process occurs as a natural part of aging, certain factors can influence when and how intensely you experience it. The primary cause is the decline in estrogen and progesterone levels, but lifestyle, genetics, and medical conditions (such as hysterectomy or chemotherapy) can also play a role. Smoking and high-stress levels may even trigger earlier or more severe perimenopausal symptoms.
Symptoms
Perimenopause symptoms vary widely from person to person. Some of the most common include:
- Irregular periods (heavier, lighter, or missed cycles)
- Hot flashes and night sweats
- Mood changes, anxiety, or depression
- Sleep disturbances and fatigue
- Vaginal dryness and discomfort during sex
- Decreased libido
- Weight gain
- Brain fog and memory issues
Everyone’s experience during perimenopause can vary with these symptoms, and the intensity can change over time.
How to Handle Perimenopause (and what to do about it)
Diagnosis
While there isn’t a specific test to confirm perimenopause, doctors will typically make an informal diagnosis based on your symptoms, age, and menstrual history. In some cases, they may even do blood tests to see where your hormone levels are at.
Agudelo adds, “There’s an important distinction here that’s worth calling out, and that is that perimenopause is a normal process, just like puberty, that all of us will go through. As such, there’s nothing to [formally] diagnose because it’s not a medical condition and rather, it’s about recognizing the signs that indicate we are in this transitional phase of life.”
Treatment
“Perimenopause isn’t something you have to put up with and deal with,” Agudelo says. “There are options available that can be tailored to your experience and preference. Options include hormone therapy, lifestyle changes, or non-hormonal options. More practitioners are becoming specialized in helping women navigate perimenopause.”
Treatment for the symptoms can depend on how intense your symptoms are and what solutions work best for your body. Some of the more common approaches include:
- Lifestyle changes: Following a balanced diet, regular exercise, and using stress management techniques can help ease symptoms.
- Hormone therapy (HT): Low-dose estrogen therapy can relieve hot flashes and vaginal dryness.
- Non-hormonal medications: Antidepressants, certain blood pressure medications, and other drugs can help with specific symptoms.
- Supplements and alternative therapies: HUM has supplements with natural ingredients to support hormone health and perimenopause relief for the uncomfortable symptoms that come with the transition. HUM’s Hormone Balance contains Chaste Berry and Dong Quai which can help with PMS symptoms including mood swings and irritability. However, if you’re looking for something geared a little more specific toward perimenopause/menopause relief, Fan Club’s probiotic formula targets 11 symptoms associated with the transition.
Percentage of participants taking Fan Club and their changes at 4 weeks:
- 90% had a decrease in at least 1 menopausal symptom
- 87% had fewer hot flashes
- 58% had reduced feelings of heart racing
- 62% felt less restless
- 52% had less severe mood swings
- 64% felt less irritable
- 62% felt less exhaustion
- 72% had sex drive improvements
- 49% had less bladder problems
- 49% had less vaginal dryness
- 39% had less join and muscle discomfort
- 64% had less sleep problems
- +slept on average 48 minutes longer
Perimenopause FAQs
How long does perimenopause last?
Perimenopause can last anywhere from a few months to 10 years, with the average being about four years. However, it officially ends when menopause begins (12 months without a period).
Can you still get pregnant during perimenopause?
“Yes, you can still get pregnant during perimenopause,” Agudelo states. “While it’s true that you are not in your peak fertile years, pregnancy is possible in any cycle with ovulation, even when our cycles are not perfect.”
Can I delay menopause or perimenopause symptoms?
While you can’t stop menopause, you may be able to delay its onset by maintaining a healthy lifestyle. Regular exercise, a diet rich in whole foods, and managing stress can all support hormone balance and ease symptoms.
Should I see a doctor for perimenopause symptoms?
If symptoms are affecting your quality of life—like severe mood swings, extreme fatigue, or very heavy periods—it’s a good idea to see a doctor. They can help determine the best treatment options for you.
Can perimenopause make PMS worse?
Many women find that PMS symptoms become more intense or unpredictable during perimenopause. This is due to fluctuating hormone levels. Managing stress, exercising, and tracking your cycle may help alleviate severe symptoms.
The “What is Perimenopause” Takeaway
Perimenopause is a natural yet often challenging phase of a woman’s life. However, this doesn’t mean that you have to suffer through it. While it may feel overwhelming at times, understanding what’s happening in your body can make all the difference. Being able to recognize the symptoms, explore treatment options, and make the appropriate lifestyle adjustments can help navigate this transition with greater ease. Whether it’s seeking support from a healthcare professional, connecting with others going through the same experience, or simply giving yourself grace, you don’t have to go through perimenopause alone. With the proper knowledge and tools, you can take control of your health and embrace this new chapter with confidence.
The post Perimenopause Explained: The Best Supplements and How to Ease Symptoms appeared first on HUM Nutrition Blog.
]]>The post Happy Gut, Happy Hormones? The Link Between Your Gut Health and Hormones appeared first on HUM Nutrition Blog.
]]>There’s also an intricate collaboration between your gut and hormonal regulation. “It is kind of like a well-organized team, with the microbiome that is residing in your gut as the main director with the primary job of digestion and the microbiome taking on the crucial task of influencing hormones,” says functional nutritional therapy practitioner Tansy Rodgers, FNTP.

Cortisol, estrogen and the gut
For starters, the gut helps manage cortisol levels, which deal with stress, aids in creating serotonin for mood balance, and improves insulin sensitivity for better control of blood sugar, she explains. “The gut also collaborates with thyroid function, a key player in your body’s energy regulation, and participates in the processing of estrogen, essential for hormonal balance.”
Women, in particular, have estrogen, which plays a role in everything from reproductive and bone health to menstrual cycles, sleep and even mental health. Imbalances in estrogen levels can lead to a host of issues, including heavy, crampy periods, mood swings, increased risk of fractures, poor sleep, and even risk of certain cancers, warns Anna Bohnengel, MS, RD, LD a nutritionist who specializes in fertility care.
“Bacteria that reside in the gut help with the breakdown and excretion of excess estrogen,” she says. “What’s referred to as the ‘estrobolome’ helps metabolize estrogen, ensuring its proper elimination from the body—and disruptions in gut health can hinder this process, leading to estrogen excess.”
Consider amping up for your supplement routine with these best gut health supplements from us, HUM Nutrition.
“The stress hormone”
Another key hormone that can be directly influenced by the gut is “the stress hormone” cortisol. While cortisol plays an important role in enhancing your performance and stimulating immune response, Bohnengel warns that excessive amounts of cortisol can actually wreak havoc throughout your body. “Interestingly, the gut microbiome also influences cortisol metabolism, impacting how efficiently your body clears this hormone,” she says. “An imbalance in gut bacteria can exacerbate cortisol dysregulation, contributing to symptoms like weight gain, fatigue, poor sleep and anxiety.”
It’s safe to say that keeping your gut healthy will help you in more ways than just avoiding tummy troubles. Here are some key signs to look out for that may indicate that your gut—and your hormones—may be out of balance. Plus, the best gut health supplements to take along the way!
You’re bloated
If you feel bloated here and there, that’s not uncommon; however, if it starts to become a chronic issue, it could signal a more problematic issue related to your gut. “As the food travels through the digestive tract, it is meant to be fully broken down into its component parts by the time it reaches the intestines, but sometimes food particles aren’t completely broken down, which results in fermentation in the gut producing gas and bloating,” explains Canada-based naturopathic doctor and birth doula Sarah Connors, N.D. “Since hormones are mostly built in the body from other molecules, many of which come from the diet, hormone synthesis could become compromised if nutrients aren’t being absorbed properly.” Addressing the underlying cause of the bloating, she notes, could help improve the health of the gut and, by extension, hormone health.
The best gut health supplement for bloat, by far, is HUM’s Flatter Me!
You’re constipated
Constipation is another gut-related issue that happens now and then. But, like bloating, if it’s chronic there’s almost always a root cause such as not eating enough dietary fiber or drinking enough water. If left unchecked, constipation can negatively impact your detoxification pathways, warns Jenna Volpe, RDN, LD, CLT, gut health dietitian nutritionist, which may eventually also lead to inflammation and hormonal imbalance if left unchecked. “Drinking plenty of water is a helpful way to keep things moving as well as eating fiber-rich foods like fresh fruits, veggies, whole grains, and functional foods like ground flax seeds and chia seeds,” she says. “Eating at least 3 to 5 servings of veggies per day, opting for whole vs. refined grains, and incorporating a few tablespoons of ground flax and/or chia seeds into oatmeal or a smoothie can go a long way to optimize bowel movements.”
(Need a little poop boost? Try HUM’s Celery Juice Fiber Gummies!)
You’re experiencing loose stools or diarrhea
Loose stools can be related to certain medications or viruses, but they’re more often than not the result of poor digestion and/or nutritional malabsorption that’s the result of gut microbial imbalance, overgrowth of harmful pathogens, nervous system dysregulation, digestive insufficiency, and/or some kind of inflammation in the gut lining, warns Volpe. “When it comes to diarrhea, the first step should be pinpointing the root causes of why it’s happening—not just on the surface level of symptom management, but also in terms of clinical diagnosis and even on a functional level,” she says. “Once the root cause(s) of diarrhea have been pinpointed, it becomes easier to figure out which foods are triggering symptoms and how to bring things back into balance.”
You have certain food intolerances
It’s common for certain food intolerances or sensitivity to lead to gastrointestinal symptoms such as gas, bloating, cramping and/or diarrhea. While these food intolerances may seem like the norm these days, they’re often a sign that something is off balance in the gut whether it be in the gut lining, gut microbiome, nervous system, other digestive organs (liver, gallbladder, pancreas), or even in the immune system within the gut-associated lymphoid tissue (GALT), explains Volpe.
“Leaving food intolerances and food sensitivities unchecked can impair nutritional status and detoxification, which negatively impacts all systems of the body on some level,” she says. She recommends consulting qualified healthcare providers to determine not just which foods are triggering symptoms but also to figure out what’s causing the adverse food reactions on a root-cause level. “This is usually done through a combination of food-symptom journaling, clinical testing, and functional nutrition lab testing,” she adds.

You’re super moody
There’s a reason why the gut is often referred to as the “second brain” and it’s because it contains a complex network of neurons known as the enteric nervous system (ENS), which operates independently of the central nervous system (CNS) yet it still communicates with the vagus nerve that plays a vital role in regulating many essential bodily functions. Did you know that an estimated 95 percent of the feel-good hormone serotonin is produced in your gut? As such, disruptions in gut health can impact brain function and mood, explains Bohnengel. “If you notice frequent mood swings, anxiety, or irritability, it may be a sign that your gut-brain axis is out of balance,” she says.
Add HUM’s Hormone Balance into your daily routine. It’s a great add-to-your-lineup best gut health supplement.
You’re experiencing weight changes
Unexpected weight fluctuations might be tied to gut issues impacting metabolism, explains Rodgers. For proper hormone health, she recommends eating a balanced diet, getting regular exercise, detoxing toxins from the body, practicing mindfulness activities to decrease stress, and working on any emotional health obstacles that may be causing you stress.
You’re persistently tired
Feeling constantly tired despite adequate rest could be a sign that your gut health is compromised, warns Bohnengel. “If key nutrients, say vitamin B12 and iron, are not sufficiently absorbed from the GI tract, your cells may not be getting the oxygen and key building blocks needed to make energy,” she says. “A healthy microbiome also essential nutrients and energy molecules for the body. Imbalances in gut bacteria or poor nutrient absorption can lead to feelings of fatigue and low energy levels.”
The Takeaway…
When in doubt, consult a medical professional. But, remember, a balanced diet, strong supplement routine, plenty of sleep and stress mitigation are always ways in which you can help your gut get healthier and happier.
The post Happy Gut, Happy Hormones? The Link Between Your Gut Health and Hormones appeared first on HUM Nutrition Blog.
]]>The post Seed Cycling: Why You Should Consider this for Your Hormone Health appeared first on HUM Nutrition Blog.
]]>“I love seed cycling as a concept and a way for women to engage in their own care and support harmony in their systems,” says naturopath doctor and owner of Meridian Medicine, Mona Fahoum, ND. “There is [almost] no research on seed cycling, but from a traditional medicine perspective and nutrition perspective of the seeds we use, it weaves in very nicely to support the whole system with the right energetics and nutrition in each phase of the cycle.”
What Causes a Hormonal Imbalance?
Hormones play a crucial role in regulating our day-to-day body function, influencing everything from our metabolism to mood. However, factors such as stress, poor diet, lack of exercise, sleep, and environmental toxins can contribute to a hormonal imbalance. Experiencing an imbalance can cause a variety of issues, impacting our menstrual cycles, fertility, skin health, and mental health.
One of the primary reasons for hormonal imbalance in women is the disruption of estrogen and progesterone levels. Having too much estrogen in the body can lead to irregular menstrual cycles, mood swings, and even conditions like polycystic ovary syndrome (PCOS). On the other hand, low estrogen and progesterone levels can result in symptoms like fatigue, low libido, depression, and difficulty concentrating.
For a more balanced hormone routine, incorporate HUM’s Hormone Balance.

What is Seed Cycling and How Does It Work?
Seed cycling is a holistic and natural approach to restoring hormonal balance. The process of seed cycling involves incorporating seeds into your diet during the two main phases of your menstrual cycle (follicular and luteal) to balance and support healthy estrogen and progesterone levels. “Seed cycling allows us to increase some of the phytonutrients, oils, vitamins, and minerals that can support the phases of our cycle,” Fahoum says.
There are four seeds that are consumed during seed cycling:
Pumpkin Seeds: Pumpkin seeds are rich in omega-3 fatty acids, magnesium, and zinc, which help balance estrogen and progesterone levels. They also contain phytoestrogen, a polyphenol compound that exerts an estrogen-like effect on the body.
Flax Seeds: Flax is also rich in omega-3 fatty acids and can boost fertility and estrogen production. Additionally, flax seeds contain a high amount of a plant compound called lignans, a type of phytoestrogen (or plant compound) that mimics the structure of estrogen.
Sesame Seeds: Like flax seeds, sesame seeds also contain lignans, along with calcium, fiber, iron, and zinc. Consuming these seeds helps boost (and balance) progesterone production while preventing excess estrogen from accumulating.
Sunflower Seeds: Sunflower seeds are rich in Vitamin E and selenium, which increase progesterone production and detox any extra estrogen your body may be making that you don’t need.
Before beginning the seed cycling process, understanding how the two main phases of your menstrual cycle works is fundamental to achieve a healthy balance.
Follicular Phase
The follicular phase begins on the first day of menstruation and lasts until ovulation (14 days). During this phase, it’s recommended that you consume two tablespoons of flaxseeds and pumpkin seeds each day. Using the two seeds helps estrogen levels rise during the follicular phase, peaking just before ovulation and resulting in a healthy hormonal balance. Fahoum says, “Using ground flax, for example, in the follicular phase (Days 1-14) supports mitigating any excess estrogen in the system since a good quality flax is high in lignans. That phytonutrient is a natural phytoestrogen, so it helps either lower excess estrogen (often the case in PMS) or raise low estrogen (like in menopause) –it’s a balancer.”
Luteal Phase
The luteal phase occurs after ovulation and continues until the start of the next menstrual cycle (14 days). During this phase, two tablespoons of sesame and sunflower seeds are consumed daily, providing the necessary nutrients to support progesterone production. Progesterone is the dominant hormone during this phase; sunflower and sesame seeds help progesterone levels rise while slowly lowering your estrogen levels, balancing both hormones. Zinc, for example, which is largely found in sesame seeds, Fahoum says, “has been shown to concentrate and support the corpus luteum, which is responsible for progesterone production in the luteal phase.”
How Does Seed Cycling Benefit the Body?
While scientific evidence regarding seed cycling is almost non-existent, a recent study found that using seeds to treat polycystic ovary syndrome (PCOS) may prove the concept works. The study examined 90 women with PCOS, between ages 15 and 40 years old, for 12 weeks and divided them into three groups:
- The first group was a control group.
- The second group was an experimental group that treated the women with a portion-control diet and a 500mg dose of Metformin daily.
- The third group was also an experimental group that treated the women with a combination of a portion-control diet and seed cycling.
After 12 weeks, results showed that the highest follicle-stimulating hormone (FSH) levels were found in the control group, followed by the second group, with the seed cycling group showing the lowest levels (a 1.2%-2.5% decrease). As for the Luteinizing hormone (LH), levels in the control group showed an increase, while both experimental groups showed a decline. Specifically, the seed cycling group showed a decrease of 1.5%-2%. Overall, the study concluded that incorporating seed cycling into a woman’s diet can help treat PCOS.
Here are other benefits of incorporating seed cycling:
1. Balancing Hormones Naturally
The main benefit of seed cycling is its ability to naturally balance estrogen and progesterone levels within the body. The specific nutrients found in these four seeds support the body’s natural hormone production, helping to restore any hormonal imbalances.
2. Menstrual Cycle Regularity
Seed cycling is often praised for its potential to regulate menstrual cycles. Synchronizing the recommended seed intake with the two main phases of your menstrual cycle increases the chance of having regular periods on a stable schedule. This regularity can, in turn, alleviate symptoms associated with irregular cycles, such as mood swings, bloating, and cramps.
3. Reduced PMS Symptoms
Those who suffer from premenstrual syndrome (PMS) can experience symptoms ranging from irritability to fatigue and even breast tenderness. The balanced hormonal support from seed cycling can reduce the severity of PMS symptoms, enhancing overall well-being during the menstrual cycle.
4. Improved Fertility
For those trying to conceive, hormonal balance is the foundation for a healthy conception. During the menstrual cycle, your body creates and releases an egg in preparation for fertilization. If the egg isn’t used, your uterine lining sheds, resulting in you getting your period. In addition to the benefits of having regular menstrual cycles with healthily balanced hormones, seed cycling can increase the chances of fertility and conception.
5. Enhanced Skin Health
Hormonal imbalances can often negatively affect the skin, contributing to conditions like acne and dryness. The hormone-balancing properties in seed cycling, such as Vitamin E, zinc, and omega-3 fatty acids, can promote a clearer complexion and a more radiant appearance.
How to Start Seed Cycling
Achieving positive results from seed cycling and balance hormones requires planning, consistency, and patience. This step-by-step guide will teach you how to incorporate seed cycling into your routine:
- Familiarize Yourself with Your Menstrual Cycle
Start by tracking your menstrual cycle to determine the length of your follicular and luteal phases. Doing this will help you properly sync seed cycling with your body’s natural rhythm.
- Stock up on Your Seeds
If you don’t already have them at home, make sure to purchase all of the seeds you will need. Choose high-quality flaxseeds, pumpkin seeds, sesame seeds, and sunflower seeds for the seed cycling process. (Pro Tip: Using ground flax seeds as an alternative to whole seeds can offer more nutritional benefits since they’re easier to digest.)
- Incorporate the Seeds into Your Diet
During the follicular phase (days 1 through 14), consume two tablespoons (each) of ground flaxseeds and pumpkin seeds daily. As you enter the luteal phase (days 14 through 28), consume two tablespoons each of sesame and sunflower seeds. You can incorporate the seeds into your daily meals by adding them to smoothies, salads, yogurt, or oatmeal.
- Be Patient and Consistent
Balancing your hormones to healthy levels doesn’t happen overnight; therefore, being patient and consistent with your seed cycling routine is essential. Fahoum states, “I always tell my patients — ‘We didn’t get here in one day, so we’re not going to resolve it tomorrow.’ Our cycles are about a month long and in order to get our hormones to harmonize again, our bodies literally have to clean out old instruments, build, fix and retune. I expect improvements to start occurring within the first couple cycles.”
- Monitor Your Results and Adjust as Necessary
Just as it’s important to be patient and consistent, it’s also necessary to regularly assess how your body responds to seed cycling. If you notice positive changes with the incorporation of the seeds, such as improved energy levels, regulated menstrual cycles, and reduced PMS symptoms, continue with the routine. If you experience adverse effects or see no results, consider seeing a naturopath physician to discuss specialized care.
Seed cycling provides a nutritional and holistic approach to hormonal balance, addressing the root causes of imbalances rather than masking the symptoms like many medications can. By incorporating specific seeds into your diet during different phases of your menstrual cycle, you can naturally support the production of estrogen and progesterone, leading to consistent menstrual cycles, reduced PMS symptoms, and enhanced overall well-being. While seed cycling is natural and generally safe for most individuals, it’s essential to consult with your healthcare provider before starting a new treatment, especially if you have any underlying health conditions or concerns.
The post Seed Cycling: Why You Should Consider this for Your Hormone Health appeared first on HUM Nutrition Blog.
]]>The post Menopause Does WHAT to Your Sleep?! appeared first on HUM Nutrition Blog.
]]>Of course, getting enough sleep remains an essential piece of your health and wellness, so addressing barriers is important. Understanding how menopause affects sleep can help you prepare and incorporate habits to set yourself up for success.

Menopause and Sleep: The Connection
Sleep issues become more common as women get older. Evidence suggests that approximately 40-50% of perimenopausal women experience sleep disorders and this number can rise to as high as 60% among postmenopausal women.
Why? Menopause comes with a few of its own specific sleep-disrupting characteristics. Many women experience insomnia, hot flashes, and sleep-disordered breathing that makes it difficult to consistently get rest. And understandably so — nobody rests well when they’re overheating, breathing abnormally, or awake into the wee hours of the night for no apparent reason.
As for the underlying causes, we can mostly blame the fluctuating hormones. Menopause is literally the pausing of the menstrual cycle. During this season of life, your ovaries stop producing estrogen and progesterone. These two hormones are heavily involved in your appetite, mood, sex drive, sleep, body temperature regulation, and even your breathing rate — so no wonder all of these things are affected.
Not getting enough sleep is annoying and impacts every aspect of your life beyond bedtime. Adequate sleep is critical for your ability to focus and think clearly, have the energy to engage in your daily activities, for your immune health, and for your long-term wellness.
Now that you know how menopause affects sleep, what can you do about it? Let’s dive into some potential options.
All-Natural Remedies for Better Sleep
The best approach for improving menopausal sleep is to incorporate consistent everyday habits that may help ease symptom severity.
One way to do this is by incorporating natural remedies. While Western medicine and pharmaceuticals certainly have a place in getting through menopause, natural remedies may help alleviate certain symptoms.
Lifestyle Changes to Improve Sleep
Consider what your typical day-to-day routine looks like and identify some areas where improvements could be made to better support your sleep.
Three of the most impactful lifestyle habits include:
- Exercise: A 2022 review found that exercise intervention can be successful in improving insomnia among menopausal women, especially if you have an existing sleep disorder. Consider what types of activity you enjoy doing and carve out time to move intentionally for at least 30-60 minutes most days. Perhaps a combination of swimming, biking, jogging, walking, group fitness, or tennis.
- Stress management: If you’ve ever tried to go to sleep after a stressful event, you know that calming your mind can feel impossible. Incorporating stress management techniques into your regular routine can help. Keep a journal next to your bed, where you can do a “brain dump” at night and release things you’re worried about. Listening to music, stretching and yoga, meditation, and breathing techniques can also be helpful.
- Sleep environment: To promote a good night’s rest, design a sleep-promoting environment. If you’re experiencing hot flashes at night, have layers on your bed that can easily be removed. Wear something breathable that won’t trap sweat. Consider a white noise machine, fan, or blackout curtains if needed.
Dietary Adjustments
Your diet can also be adjusted to better support sleep during menopause. After all, nutrition is a key component of your mental and physical health. Without the proper nutrients, your body has a harder time keeping you healthy.

Add these sleep-promoting foods to your diet:
- Tart cherry juice, which is high in melatonin, a compound produced in your brain as part of your natural circadian rhythm, and may improve sleep time and efficiency
- Walnuts, which are rich in omega-3 fatty acids that may help promote the production of serotonin, a neurotransmitter involved in sleep and mood
- Fatty fish, which are rich in omega-3s as well as vitamin D, which may help promote serotonin production and support normal sleep
- Kiwis, which may promote serotonin production and are also rich in anti-inflammatory antioxidants like vitamin C that may increase sleep duration and reduce sleep disturbances
- Almonds, which provide magnesium, a mineral involved in relaxation that may also support normal sleep
Staying hydrated is also a critical part of your menopause routine. Your body is around 60% water at any given time, and fluid is regularly lost through normal processes like urination, sweating, and other daily maintenance. It’s important to replenish your fluids for proper temperature regulation and immune function.
If you struggle to stay hydrated, consider these tips:
- Fill a reusable water bottle in the morning to take with you
- If you get bored of plain water, add fresh lemon or cucumber slices for natural flavoring, or try unsweetened seltzer water
- Start your day with a glass of water versus drinking a bunch at night, as the latter may disrupt your sleep due to trips to the bathroom
Herbal Supplements
Many women find that adding herbal supplements to their sleep routine can help them achieve better rest at night. Some of these include:
- Valerian root, which contains an active compound called valerenic acid, which is responsible for its sedative effects
- Lavender, a flowering plant in the mint family that may have anti-anxiety, sedative, and brain-protective properties
- Passionflower, which offers anti-anxiety, sedative, and mood-supportive benefits
- Turmeric, an Indian spice with the bioactive component curcumin, which offers anti-inflammatory and antioxidant effects and supports brain health
Note that herbal supplements aren’t for everyone and can interact with certain medications and other supplements. Speak with your healthcare provider before adding these to your sleep regimen.
Calming Nighttime Drink Recipes
Sometimes, starting your nighttime routine with a warm, soothing beverage can help set you up for better sleep success. Here are three recipes that are not only simple and tasty but also contain ingredients that may help prepare your mind and body for rest.

Herbal Sleep Tea
Ingredients
- 1 tsp dried passionflower
- 1 tsp dried lemon balm
- 1 tsp dried chamomile
- Boiling water
- Optional: honey or other sweetening agent
Preparation
Combine your dried herbs together in a tea ball or reusable tea bag and place it in your mug. Add boiling water to fill your mug and allow your tea to steep for 3-5 minutes or per your liking. Remove your tea bag from the water and gently mix in your desired sweetening. Serve.
Golden Milk
Ingredients
- 1 cup unsweetened plain soy milk
- ½ tsp ground ginger
- ½ tsp ground turmeric
- ½ tsp ground cinnamon
- 1 Tbsp unsweetened cashew butter
- Pinch of black pepper (to help boost the absorption of curcumin from the turmeric)
- Optional: sweetener of choice
Preparation
Combine all of your ingredients in a saucepan and whisk them together while heating over medium heat. Continue to stir gently and heat for 3-5 minutes until well combined and warmed throughout. Serve.
Lavender Chamomile Infusion
Ingredients
- 1 tsp dried chamomile
- ½ tsp dried lavender
- Optional: ½ tsp dried mint, sweetening agent
- Boiling water
Preparation
Combine your dried herbs (and optional mint) in a tea ball or reusable tea bag and place it into your mug. Fill your mug with boiling water. Allow herbs to steep for 3-5 minutes before removing. Add an optional sweetening agent and serve.
Incorporating HUM Products
In addition to products designed to help support your overall health and wellness, HUM also makes some that may be particularly beneficial for menopausal support, like:
Berberine is a plant compound found in things like European barberry and goldenseal. Designed to be taken daily with food, our berberine capsules help support the body’s glucose and fat metabolism for healthy glucose and cholesterol levels*. They contain BioPerine®, a patented piperine derived from black pepper that helps nutrient absorption*. Additionally, berberine supports beneficial bacteria and promotes a healthy gut microbiome.
This daily capsule is an estrogen-free, non-hormonal, clinically studied probiotic formula that addresses 11 symptoms of perimenopause and menopause. It features ingredients like Siberian rhubarb extract to reduce the severity of hot flashes, night sweats, vaginal dryness, fatigue, and irritability, patented probiotics to support the gut-brain axis and mood, and grape seed extract for stress support.
Be sure to consult with your healthcare professional before adding any new supplements to your routine, to ensure that they are safe and appropriate for you.
Rest Easier During Menopause
Sleep is an essential element to your quality of life and everyday health. Unfortunately, getting enough of it on a consistent basis is easier said than done during menopause. When you’re experiencing side effects of such dramatic hormonal changes, like hot flashes, night sweats, and insomnia, it’s difficult to find restful sleep.
The good news is that there are everyday habits and dietary changes that may be helpful. Explore natural remedies and calming drinks to see what helps you. Consider adding a HUM product like Best of Berberine or Fan Club to help support your best health and rejuvenation during menopause.
to help support your best health and rejuvenation during menopause.
The post Menopause Does WHAT to Your Sleep?! appeared first on HUM Nutrition Blog.
]]>The post Snack Your Way To Better Hormone Balance appeared first on HUM Nutrition Blog.
]]>You’ve got hormones—lots of them. Your endocrine, or hormonal, system is complex, hosting at least 50 hormones that affect everything from blood sugar balance, to fertility, energy production, and more. And, it’s become buzzy on social to take steps to correct a hormonal imbalance with hormone-balancing foods so your body can function at its best.
Certainly, an overall healthy diet is key, but it always helps to hone in on specific foods that support hormonal health. While you clearly have dozens of hormones coursing through your body, we’re specifically focused on female sex hormones, estrogen, progesterone, and androgens (such as testosterone) in this article.
When Hormones Get Whacky
When these hormones are out of whack, you may experience period problems, such as irregular cycles, PMS symptoms, headaches, mood changes, and breast tenderness that arises around your period, says Melissa Grobess Azzaro, RDN, founder of The Hormone Dietitian.
The thing is, “hormones don’t become imbalanced on their own,” says Azzaro. “Hormonal changes are caused by something going on upstream, which affects hormone levels downstream,” she explains. Those upstream factors include:
- Blood sugar imbalances and insulin dysregulation
- Inflammation
- Excess stress
- Not enough sleep
- Under-eating for your activity level
- Environmental exposure to endocrine-disrupting chemicals
So, how to balance hormones? We’ve rounded up some delicious, nutrient-packed between-meal bites that deliver on that promise. These foods target many of the upstream factors that lead to hormonal issues. Here are the best snacks for hormone balance—hopefully you can enjoy one today.
Hormone-Balancing Snacks and Their Benefits
When you’re feeling snacky, you have a lot of options. But traditional choices—we’re looking at you chips, and pretzels—doesn’t really cut it when it comes to your hormones. The goal is to consume snacks that are made from whole, minimally processed foods that help manage your blood sugar, offer antioxidants to wipe the negative effects of inflammation, and may also impact sex hormones in direct ways.
These may include:
- Nuts and seeds make fantastic choices for supporting hormonal health, says Azzaro. “All are high in healthy fats, protein, fiber, vitamins and minerals, which are needed to help support the body’s natural detox pathways,” she explains. Healthy fat and protein support steady blood sugar levels. In addition, minerals like magnesium and vitamins like the B vitamins help the body with hormone metabolism, she explains.
- Fruit provides antioxidants that decreases inflammation, a stressor on the body. Certain fruits can also aid in estrogen regulation and help increase progesterone levels.
- Other foods, such as full-fat yogurt, cruciferous vegetables, dark chocolate and more, which support fertility and proper estrogen levels, as well as provide specific nutrients that assist in insulin function.
Seed-Based Snacks for Hormone Balance
It’s a good idea to eat a variety of nuts and seeds regularly rather than focusing on one or two power players. That’s because they each provide slightly different nutrient profiles. For example:
- Brazil nuts are an excellent source of selenium, a mineral needed for thyroid function.
- Pumpkin seeds are rich in zinc, a mineral that one meta-analysis in the journal Nutrients shows that this nutrient can help quell period pain, and PCOS symptoms.
- Flaxseeds are “one that I recommend that most women eat every day from when they start their period in youth to menopause,” says Azzaro. Flax contains phytoestrogens, which are estrogen-like compounds in plants, which can help regulate estrogen levels. In addition, flax has soluble fiber that can bind to excess estrogen and help eliminate it, she explains. Choose ground flaxseeds, which are easier to digest. Flax can be sprinkled on yogurt or oatmeal or added as an ingredient to an energy ball.

Fruit-Based Snacks for Hormone Balance
Though all fruit is healthy, Azzaro specifically recommends those like berries and citrus fruit for hormone-balancing snacks.
- Berries are high in fiber and antioxidants, says Azzaro. Fiber helps the body eliminate excess estrogen while antioxidants help counteract inflammation.
- Citrus fruit is also high in antioxidants, but also vitamin C, a vitamin that may help increase progesterone levels, according to the Cleveland Clinic.
- Kiwi is not only bursting with vitamin C, but the fruit contains melatonin (a sleep-regulating hormone), serotonin (a feel-good hormone that also improves sleep, and antioxidants (to decrease inflammation), according to 2023 research.
- Avocado supplies a good source of heart-healthy monounsaturated fatty acids. “We need enough calories and fat to make hormones in the first place,” says Azzaro. Avocado is a fruit, though one that’s rich in these fats. Smearing avocado on a piece of whole grain toast and topping with a whole egg is a really satisfying snack.
For traditional fruits (like berries and citrus), Azzaro recommends pairing your fruit with a source of protein. Fruit is a source of nutrient-rich carbohydrates, but for optimal blood sugar balance, “it’s not a good idea to eat carbohydrates alone, even if it is healthy like fruit,” she says. So, pair a fruit with a piece of cheese, some nuts, or yogurt.
Why? Blood sugar affects insulin, another hormone. When your blood sugar spikes, which can happen when you eat carbohydrates alone, your body interprets that rise and fall as a source of stress, which can tax your adrenal glands. Your adrenals are what pumps out stress hormones, like cortisol, as well as play a role in estrogen and testosterone production, notes the National Library of Medicine.
“When we talk about minimizing stress, this doesn’t just refer to psychological stress, but physical stressors as well, such as having imbalanced blood sugars or inflammation,” says Azzaro. “These internal sources of stress can throw your adrenal hormones off balance, which has downstream effects on your sex hormones,” she explains.

Other Nutrient-Dense Snacks for Hormone Balance
You don’t have to limit yourself to nuts, seeds, and fruit to give your hormones TLC. Here are four other snacks to eat:
- Yogurt, especially full-fat yogurt compared to non- or low-fat versions, has been shown to help support fertility, says Azzaro. In addition, yogurt also supplies a source of probiotics, which adds good bacteria to your gut. “Anything that supports gut health also supports hormone health,” she says. If you can’t do dairy, add some dairy-free kefir to your smoothie or go for a plant-based yogurt. One yummy idea? Top off Greek yogurt with berries and seeds for a nice crunchy texture.
- Cruciferous vegetables, such as kale, radishes, broccoli, and cauliflower are also rich in fiber. These veggies also contain compounds called glucosinolates, which may affect estrogen metabolism. This is one reason why some research suggests that eating cruciferous veggies is associated with a reduced risk of breast cancer. Dip pieces of raw veggie in hummus or guacamole.
- Salmon and olives are other sources of healthy fats that can be used in snacks, says Azzaro. In addition, salmon contains docosapentaenoic acid (DPA), a type of polyunsaturated fat associated with increases in progesterone production and proper ovulation, research shows. Pair a few olives with nuts and cheese. And don’t count out salmon when it comes to snacking. Azzaro likes a salmon snack made with a crisp bread smeared with hummus, topped with smoked salmon and cucumber.
- Dark chocolate, Not only supplies a wealth of flavonoids, plant compounds with antioxidant properties, but also magnesium. About one-quarter of women who have PCOS don’t get enough of this mineral, which is associated with insulin resistance. According to research in Current Developments in Nutrition. To turn dark chocolate into a snack, pair a couple of squares (of for at least 75% cacao) with raspberry tea, a sip that’s been used to soothe menstrual cramps.

The Takeaway
There are so many wonderful hormone-balancing foods that make great snacks. Even better: You can combine many of these—a yogurt and berry bowl, a handful of pumpkin seeds and an orange—for a well-rounded, nutrient-dense snack that supports hormonal health. Isn’t it time for a snack by now?
The post Snack Your Way To Better Hormone Balance appeared first on HUM Nutrition Blog.
]]>The post 7 Facts About Having Sex on Your Period (Some of Which May Surprise You) appeared first on HUM Nutrition Blog.
]]>If you menstruate, you know a thing or two about periods—including that they can be pesky and sometimes painful. But this monthly bleed, which typically happens every 21 to 35 days and lasts up to seven days each cycle, is actually a good thing. Its recurrence indicates that you are healthy and fertile.
Despite that nearly half of the world’s population gets a period in their lifetime—and the fact that this biological occurrence has essentially been happening since the dawn of time—there are countless myths circulating about it. This rings especially true when it comes having period sex. For example, some people think that it is a bad thing to have sex on their period and try to avoid it as a result.
Having sex on your period might be uncomfortable for some people (not to mention it may a little messier than usual). But rest assured that when you take the right precautions, it can be perfectly safe—and yes, even enjoyable. “A period is a natural thing, so there’s really no reason to hold off,” says Aimee Eyvazzadeh, MD, a San Francisco-based fertility specialist. What’s more: There may actually be some benefits of period sex you may miss out on.
Ahead, we’re sharing some of the most surprising things you perhaps never knew about having sex on your period.
First, What Is a Menstrual Period?
A menstrual period entails the shedding of the uterine lining. It occurs as the result of the female egg not becoming fertilized by sperm during that given cycle. Every month, the female body releases an egg in a process called ovulation, which lasts only 12 to 24 hours, Dr. Eyvazzadeh explains, which is also known as the menstrual process.
If the egg is not successfully fertilized by sperm within that time frame, two female sex hormones—progesterone and estrogen—start to decline. This decline is what sparks the shedding of the uterine lining (i.e., blood and tissues that were building up in case a pregnancy did occur). “Your period is essentially the process of your uterus bringing itself back to baseline to prepare for the next cycle,” she says.

7 Facts About Having Sex During Your Period
Is it “bad” to have sex on your period? Does period sex make you more attached? Can sex delay your period from coming? Discover answers to these pressing questions, plus additional FYIs and benefits of period sex.
1. You May Experience Less Cramping
As many as 84.1 percent of women who menstruate experience period pain, per a study published in the Journal of Pain Research. It is an incredibly common symptom along with many others such as:
- bloating
- breast tenderness
- mood swings
- irritability
Despite what you might think, having sex on your period can actually help alleviate period discomfort—especially if you experience orgasm during intercourse. “During orgasm, the uterus contracts, which may help relieve cramps,” explains Lauren Demosthenes, MD, senior medical director at Babyscripts. “Additionally, the feel-good endorphins that are released with pleasure, including dopamine, may help.”
2. Sex Won’t Delay Your Period
Menstrual cycles are regulated by a woman’s brain (specifically her pituitary). That said, you don’t have to worry about sex delaying your period in any way, according to Natalie Stentz, MD, a double board certified OB-GYN and fertility specialist. “The activity of penetrative intercourse may make menstrual blood more apparent by bringing it out of the vagina, but the underlying process is totally unrelated to intercourse,” she clarifies.

3. Period Sex Might Make You Feel More Attached
If you are curious if emotional attachment can be enhanced by your period, you are onto something. Due to the increased arousal that you can feel during your period, it’s quite likely that you might feel stronger emotions towards your sex partner. While this is certainly no reason to avoid having sex on your period, it definitely pays to keep this in mind if you’re worried about developing feelings of attachment. Moreover, it could very well be a good thing to promote greater intimacy with your significant other.
4. You May Need to Use Lube During Period Sex
You might think that the last thing you would need to have sex during your period would be extra lubrication. However, Allison Rodgers, MD, an OB-GYN and reproductive endocrinologist at Fertility Centers of Illinois, points out that estrogen—which is responsible for keeping you lubricated down there—is actually quite low around your period. (Remember how we explained that your hormone levels take a dip when you don’t successfully conceive?) As a result, you may need some help with lubrication, particularly if you’re having sex towards the end of your period.
5. It’s Possible to Get Pregnant on Your Period
Some couples using natural methods of birth control will try to have sex at certain times in the woman’s cycle when they believe they are less likely to get pregnant. While it is true that the timeframe of when your body sheds its uterine lining is an unlikely time to conceive, it is not impossible.
Again, most periods occur every 21 to 35 days, but some fall outside of this range. Some are also irregular and don’t follow a predictable pattern from month to month. Also, irregular vaginal bleeding may be mistaken as a true menstrual withdrawal bleed, says Mark Trolice, MD, an infertility specialist at Florida’s Fertility Care IVF Center.
“Bleeding can occur for other reasons unrelated to ovulation, such as an ovarian cyst, polycystic ovary syndrome (PCOS, the most common hormonal imbalance in women), uterine polyps, or fibroids (benign growth in the uterus),” he explains. “So ovulation can occur during vaginal bleeding that can be mistaken for a real period. As a result, pregnancy can occur during this ‘false’ period.”
Additionally, sperm can live up to five days within the vagina, per a study published in Advanced Contraception. Hence, it is possible to get pregnant five days prior to ovulation. For those who have a shorter cycle, they may still bleed during those five days prior to their next ovulation.
6. Period Sex Doesn’t Have to Be Messy
One of the biggest reasons couples avoid sex when one person is on their period is due to the mess that they think will result. However, the bleeding that occurs during menstruation is quite slow. In fact, per the NIH, it takes about four hours for the average person to soak a regular tampon.
What’s more: Dr. Eyvazzadeh notes that you can have a totally mess-free period sex if you use a menstrual disc, or a flexible cup made of silicone or latex that sits in the vagina and collects blood. “The male partner usually can’t tell it is in, and the female partner doesn’t have to worry about possible stained sheets or bleeding on her partner so can enjoy the act more,” she says.
7. Having Sex During Your Period Won’t Make It More Likely to Get an STI
Research has long weighed in on whether or not having sex on one’s period could increase the risk of contracting a sexually transmitted infection. However, there is little evidence to support this, says Dr. Stentz. “More recent studies suggest that couples are no more likely to contract HIV or pelvic inflammatory disease from menstrual intercourse,” she explains. “That said, outside of a strictly monogamous relationship, it is always important to use barrier contraception as a preventative against sexually transmitted infections.”
The Emotional Considerations of Period Sex
Having sex on your period with your partner can actually lead to a more intimate and deep bond. Some feel a spiritual effect of having sex during menstruation. This can be due to the vulnerability it takes to come together in an intimate act while a woman is in the middle of her menstruation.
Period Sex FAQs
Can having sex during your period shorten its duration?
Sex during menstruation may help shorten its duration slightly by causing uterine contractions, which can help expel menstrual blood more quickly.
Is it safe to have oral sex during menstruation?
Yes, it’s generally safe to have oral sex during menstruation, but using protection like a dental dam can reduce the risk of exposure to bloodborne infections.
What are the best sexual positions to minimize mess during period sex?
Positions like spooning or lying on your side can help minimize mess by keeping the flow contained and reducing movement.
How can I talk to my partner about having sex during my period?
Approach the topic openly and honestly, expressing your comfort level and asking for their thoughts to ensure mutual consent and understanding.
Are there any health conditions that make period sex unsafe?
Certain conditions, like sexually transmitted infections or heavy menstrual bleeding, may require caution or medical advice before engaging in period sex.
Can period sex alleviate PMS symptoms?
Yes, period sex may help relieve cramps and mood swings due to the release of endorphins and muscle relaxation from orgasms.
What hygiene practices should be followed before and after period sex?
Both partners should wash their hands and genitals before and after sex, and using a towel or menstrual cup can help manage mess.
Does menstrual blood act as a natural lubricant during sex?
Menstrual blood can provide some lubrication, but it might not be sufficient for everyone, so additional lubricant may still be needed.
Can period sex affect the regularity of my menstrual cycle?
No, having sex during your period does not typically affect the regularity of your menstrual cycle.
Is it normal to feel increased sexual desire during menstruation?
Yes, hormonal changes during menstruation can lead to heightened sexual desire for some individuals.
The bottom line: Safe sex always matters, whether or not you are on your period.
The post 7 Facts About Having Sex on Your Period (Some of Which May Surprise You) appeared first on HUM Nutrition Blog.
]]>The post Are These Hunger Hormones Sabotaging Your Diet and Weight Loss Goals? appeared first on HUM Nutrition Blog.
]]>When you hear “hormones,” your brain might immediately jump to your period, or maybe melatonin. BTW, hormones are your body’s powerful chemical messengers, and there are over 50 known hormones pumped out by our endocrine system. They play a vital role in everything from growth and reproduction to mood and sleep.
Hormones also impact metabolism and appetite—and that’s where ghrelin and leptin come in.
“Optimal health is related to these ‘hunger hormones’ and your metabolic reaction to the foods you eat,” says Florence Comite, MD, an endocrinologist and the founder of the Comite Center for Precision Medicine and Health in New York City, Miami Beach, Florida and Palo Alto, California.
Together, leptin and ghrelin regulate our sensations of hunger and satiety by sending signals to our brain, adds Ammara Aziz, MD, an endocrinologist with Northwest Community Healthcare in Arlington Heights, Illinois. When these power players are balanced, our bodies are better able to maintain a consistent weight. Yet if things get too weighed down on one side of the ghrelin vs. leptin seesaw, your appetite and the way your body uses energy can get thrown out of whack.
Ahead, learn more about ghrelin and leptin, including how to tell if your levels might fall outside of the “normal” range. And later: simple strategies you can try today to support balanced hunger hormones.
What Is Ghrelin?
Ghrelin is a hormone produced mainly by the stomach. Small amounts are also released by the small intestine, pancreas and brain, Dr. Aziz explains.
“Ghrelin communicates with the brain to let it know that you’re hungry,” adds Patricia Bannan, MS, RDN, a dietitian based in Los Angeles and the author of From Burnout to Balance. “When your stomach is empty or nearing empty, it releases ghrelin. Once you eat a meal or snack and you feel satiated, ghrelin levels will fall.”
To remember that this is the main “hunger hormone,” Dr. Comite tells her patients and students to think of “grrrhelin,” like a growling stomach. Beyond stimulating appetite, ghrelin also affects carbohydrate metabolism, fat storage, blood sugar, and other processes in the body.

What Is Leptin?
You can think of leptin as the yin to ghrelin’s yang. This hormone regulates appetite and energy balance to maintain your body weight over time (in addition to other important tasks like immune function). But instead of being released by the stomach like ghrelin, leptin is emitted by our white adipose (aka fat) tissue.
“Leptin’s purpose is to tell the body that you’re full, and it plays an important role in weight maintenance. When you have adequate fuel sources and your body is satisfied, leptin levels will increase to communicate to the brain that you don’t need to consume more energy,” Bannan says. “When you’re hungry or unfed, leptin will fall.”
Since the level of leptin in our blood is directly related to how much body fat we have, higher levels of leptin are seen in individuals who live in larger bodies. Research shows that the leptin-to-ghrelin ratio tends to increase with increasing body mass index (BMI).
Over time, elevated levels of leptin can lead to leptin resistance, in which the body loses its sensitivity to the hormone. This can impact the body’s ability to experience feelings of fullness.
If rapid weight loss occurs, a decrease in leptin can trigger the body to enter what Dr. Aziz calls ‘starvation mode,’ which she says makes it difficult to lose more weight. (Psst: This is a very good sign it might be time for a reverse diet.)
“Prolonged fasting associated with intense hunger is likely due to very low leptin levels, especially with weight and fat loss,” Dr. Comite says. “Your body is saying ‘I’m starving; I’d better eat!’” This is why you may experience intense hunger pangs, cravings, or symptoms of binge eating after skipping meals, Dr. Comite continues.
How to Tell If Your Ghrelin and Leptin Levels May Be Imbalanced
“There are many factors that can impact both ghrelin and leptin levels, including genetics, body fat levels, and an energy deficit,” Bannan says.
The only way to directly assess levels of ghrelin and leptin is to get a blood test. However, Dr Aziz says that these tests are rarely performed. Hunger hormone levels are only checked in very specific cases, such as in children who fall under the classification of class III obesity.
If you’re on a calorie-restricted diet, though, cyour ghrelin levels are likely high. This is your body’s savvy way of nudging the brain to feed itself. Also, the more body fat you have, the more leptin you’ll have pumped into your bloodstream to try to cue your brain that you’re all set, so your leptin levels are likely higher.

7 Ways to Promote Healthy Hunger Hormone Levels
As of yet, scientists aren’t aware of any foods, prescriptions, or supplements that could potentially help the body to make leptin optimally to signal fullness. That said, there are several lifestyle habits that can help your leptin and ghrelin levels stay within healthy ranges.
1. Balance Your Macros
Choose meals and snacks that provide protein, carbohydrates (ideally with some fiber), and healthy fats. Doing so can support blood sugar stability, which is an important part of avoiding energy spikes and crashes as well as food cravings. “These balanced meals and snacks will also help your body regulate your natural hunger and fullness cues by supporting ghrelin and leptin balance,” Bannan says.
2. Prioritize Protein
While all three macronutrients are important, protein is the most effective at suppressing ghrelin, Dr. Comite adds. This means it’s also the most satiating macronutrient of the trio. For a 150-pound person, aiming for about 27 to 35 grams of protein per meal is a great goal to ensure you’re consuming enough protein throughout the day.
3. Fuel Regularly
Restrictive fasting is not your BFF if you’re aiming to harness the power of your natural hunger hormone patterns. “Never allow yourself to get famished. Eat at regular intervals throughout the day—about every two to four hours,” Dr. Comite advises. Each of us is unique, so experiment to determine the eating strategy that works best for your own biochemistry.
4. Load Up on Nutrient-Dense Foods
A simple way to feel full on fewer calories (if that’s the goal): Add volume to your plate. Focus on nutrient-dense yet low-calorie foods, such as:
- fruits
- vegetables
- whole grains
- lean meats
- fish
- legumes
From there, accent with healthy fats and more calorie-rich components—such as cheese or butter—in smaller quantities.

5. Stay Active
The World Health Organization, the US Department of Health and Human Services, and the American College of Sports Medicine all recommend that adults aim for 150 minutes of moderate-intensity aerobic activity per week, as well as two total-body strength training sessions.
All exercise improves leptin sensitivity, Dr. Comite says, but it’s especially important not to forget about strength. “Resistance training is key to help maintain muscle mass, which declines with age beginning in the 30s,” she explains. (Tip: Discover how to mix cardio and strength workouts for the best results.)
6. Score More Shut-Eye
Research suggests that sleep deprivation causes ghrelin to rise. Even one night of insufficient sleep can increase ghrelin and hunger levels. “In addition to having many other benefits for our health, getting an adequate amount of sleep helps prevent rises in ghrelin, which makes us feel hungrier,” Dr. Aziz says. Aim for seven to nine hours per night.
7. Practice Self-Care to Reduce Stress
According to Dr. Comite, stress might make leptin resistance more likely. To manage stress and carve out more me time, consider deep breathing, taking a walk, reading a book, or simply turning your phone to Do Not Disturb mode.
The Bottom Line
Ghrelin and leptin are two key hormones involved in our body’s appetite, food intake, and weight gain/loss. “Since we know that leptin levels decrease in response to weight loss, triggering starvation mode, it has helped us understand why weight loss becomes harder as we lose weight,” Dr. Aziz says.
But as we continue to learn more about how to harness the power of these hormones, Dr. Comite suggests looking at your body as a system—not just a set of hormones. She consults patients to look at their full picture of personal health, including their genetics as well as lifestyle habits such as sleep, food, exercise, and restorative practices like meditation. Considering total personal health in tandem with hormonal and metabolic factors, you and your doctor may be able to “predict and reverse aging and diseases that may be emerging at the cellular level and optimize your health span for life and longevity,” Dr. Comite says.
Navigating the world of hormones can be a complex battle. “Remember that you know your body best. So if you feel as though your appetite or weight fluctuations are unusual, ask your health team for guidance,” Bannan advises.
The post Are These Hunger Hormones Sabotaging Your Diet and Weight Loss Goals? appeared first on HUM Nutrition Blog.
]]>The post The Results Are In: HUM’s Fan Club Is Clinically-Proven to Decrease Menopause Symptoms in 90% of Users appeared first on HUM Nutrition Blog.
]]>The impact that menopause can have on daily life is often overlooked and women have few options to help them manage perimenopause and menopause symptoms.
To give women a natural, estrogen-free solution to help reduce 11 common symptoms of menopause and perimenopause, HUM created Fan Club. Fan Club contains three key ingredients that have individually been studied to support symptoms of menopause like hot flashes, night sweats, sleeplessness, mood swings, heart racing, and fatigue.
Fan Club’s standout ingredients are:
- Siberian rhubarb root extract
- The probiotic Lactobacillus plantarum DR7
- Grape seed extract
Together, these ingredients are a powerful tool for managing symptoms and helping women regain control of their lives during perimenopause and menopause. But just how powerful are they?
We put Fan Club to the test. Or rather, took it to the lab to get clinically-backed results.
“The ingredients we use in Fan Club have really robust evidence to support their effect of improving many menopause symptoms,” says Jennifer Martin-Biggers, PhD, MS, RDN, the VP of scientific affairs and education at HUM Nutrition. “It was important for us to support users of Fan Club with additional science to show how efficacious this can be to help relieve a variety of symptoms.”
Find out how well it performed under the microscope.
How the Study Worked
To ensure no bias in our study, we worked with an independent, third-party clinical research lab in California to perform a randomized, double-blind, placebo-controlled clinical study. The lab enrolled over 100 women experiencing menopause symptoms to participate.
The research lab adhered to clinical research ethical and legal requirements. To ensure that a clinical study is conducted ethically, an independent ethics committee, called an Institutional Review Board (IRB), reviewed the study plans to make sure it was safe and designed according to research standards.
The final study included 111 perimenopausal women with mild, moderate, or severe symptoms.
The participants were split up into two groups, either the experimental group that received Fan Club, or the control group that was given a placebo. Neither the study administrators nor the participants knew which group they were in.
Both groups were instructed to take the active or placebo supplement once daily for 8 weeks. They were given surveys to assess their symptoms at baseline, and then 30 and 60 days after beginning the supplement.
Questions in the survey were designed to assess changes in menopause symptoms including hot flash and night sweat frequency and severity of 11 total menopause symptoms, as well as hours slept.
Result Highlights
The majority of participants started to see results between three to four weeks. After four weeks of taking Fan Club once per day, the experimental group had significant improvements in symptoms.
- 90% of participants witnessed positive results
- 87% of participants had fewer hot flashes
- The number of hot flashes participants had decreased by 60%
- Participants had a 40% decrease in total symptom score
- 64% of participants had fewer sleep problems, and as a bonus, they slept on average 48 minutes longer
- 72% of participants had sex drive improvements
- 49% of participants had less vaginal dryness
- 64% of participants felt less irritable
Statistical analysis showed these results to be statistically significantly decreased among participants in the Fan Club group, compared to those in the placebo group. An evaluation of statistical significance is performed with study data to help quantify if a result is due to chance or actually a result of efficacy or performance. The statistical significance of the Fan Club study indicates the formula is clinically efficacious.
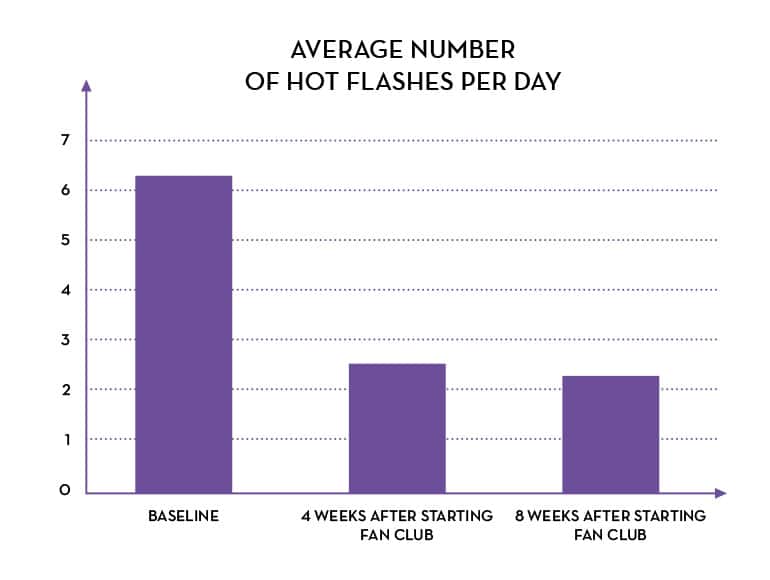
Women also reported significant decreases in the frequency and severity of other menopause symptoms including:
- Heart racing
- Joint and muscle discomfort
- Restlessness
- Mood swings
- Bladder problems
- Exhaustion
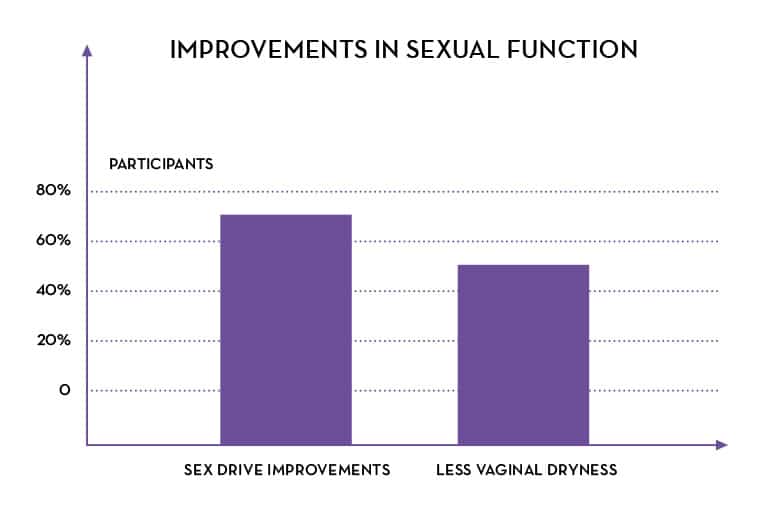
“The most impressive result is that this study tells us Fan Club starts to have a profound effect alleviating symptoms as soon as 4 weeks after taking it, and these results persist,” explains Dr. Martin-Biggers.
Throughout the course of the eight-week study, there were no adverse events reported related to Fan Club.
What Users Had to Say
While the numbers speak for themselves, we thought we’d let our trial participants do the talking, too, because their love for Fan Club is unmatched. Here’s what a few had to say about their experience after 8 weeks of taking Fan Club.

“I absolutely LOVE this product ‘cause it actually works! It has literally given my life back to me! I cannot THANK YOU enough!!!”
“I hope at the end of the test that we’re able to buy this because I’m crying happy tears just writing about this.”
“I feel very different to the way I felt 2 months ago. I have only experienced one hot flash in the past month and several other beneficial changes.”
“I no longer have hot flashes, sweating a lot, or sleeplessness. My mood and anxiety have ceased as well! My overall well-being has improved drastically!”
“I’ve tried so many different things and nothing has worked since this.”
Join the Fan Club

We’re so happy at the results of the randomized, double-blind, placebo-controlled clinical study of Fan Club, but even more, encouraged by the meaningful impact Fan Club can have on the lives of women going through perimenopause and menopause.
“I am thrilled with the results but not surprised by them as the ingredients we used have great science supporting their effectiveness,” says Dr. Martin-Biggers.
Ready to join the Fan Club with us? (We thought so!) If you’re dealing with menopausal symptoms, Fan Club is the perfect supplement to add to your daily routine, says Dr. Martin-Biggers.
The post The Results Are In: HUM’s Fan Club Is Clinically-Proven to Decrease Menopause Symptoms in 90% of Users appeared first on HUM Nutrition Blog.
]]>


















