
The post Perimenopause Explained: The Best Supplements and How to Ease Symptoms appeared first on HUM Nutrition Blog.
]]>What is Perimenopause?

Perimenopause is the transitional phase before menopause when your body gradually reduces its production of estrogen and progesterone, the key hormones that regulate your menstrual cycle. Menstrual health practitioner Michelle Agudelo states that while it can vary from person to person, perimenopause typically occurs for women in their late 30s to early or mid-40s, lasting for four to eight years on average. During perimenopause, your periods may become irregular—sometimes heavier, sometimes lighter, or even skipping months altogether. While menopause officially begins when you’ve gone 12 consecutive months without a period, perimenopause can last for several years, bringing a variety of symptoms like mood swings, sleep disturbances, and hot flashes. The Journal of Obstetrics, Gynecology, and Cancer Research estimates that vasomotor symptoms (hot flashes) occur within 75-80% of perimenopausal women. Despite these numbers, understanding this phase can help you manage the changes and feel more in control of your health.
Causes
While the perimenopause process occurs as a natural part of aging, certain factors can influence when and how intensely you experience it. The primary cause is the decline in estrogen and progesterone levels, but lifestyle, genetics, and medical conditions (such as hysterectomy or chemotherapy) can also play a role. Smoking and high-stress levels may even trigger earlier or more severe perimenopausal symptoms.
Symptoms
Perimenopause symptoms vary widely from person to person. Some of the most common include:
- Irregular periods (heavier, lighter, or missed cycles)
- Hot flashes and night sweats
- Mood changes, anxiety, or depression
- Sleep disturbances and fatigue
- Vaginal dryness and discomfort during sex
- Decreased libido
- Weight gain
- Brain fog and memory issues
Everyone’s experience during perimenopause can vary with these symptoms, and the intensity can change over time.
How to Handle Perimenopause (and what to do about it)
Diagnosis
While there isn’t a specific test to confirm perimenopause, doctors will typically make an informal diagnosis based on your symptoms, age, and menstrual history. In some cases, they may even do blood tests to see where your hormone levels are at.
Agudelo adds, “There’s an important distinction here that’s worth calling out, and that is that perimenopause is a normal process, just like puberty, that all of us will go through. As such, there’s nothing to [formally] diagnose because it’s not a medical condition and rather, it’s about recognizing the signs that indicate we are in this transitional phase of life.”
Treatment
“Perimenopause isn’t something you have to put up with and deal with,” Agudelo says. “There are options available that can be tailored to your experience and preference. Options include hormone therapy, lifestyle changes, or non-hormonal options. More practitioners are becoming specialized in helping women navigate perimenopause.”
Treatment for the symptoms can depend on how intense your symptoms are and what solutions work best for your body. Some of the more common approaches include:
- Lifestyle changes: Following a balanced diet, regular exercise, and using stress management techniques can help ease symptoms.
- Hormone therapy (HT): Low-dose estrogen therapy can relieve hot flashes and vaginal dryness.
- Non-hormonal medications: Antidepressants, certain blood pressure medications, and other drugs can help with specific symptoms.
- Supplements and alternative therapies: HUM has supplements with natural ingredients to support hormone health and perimenopause relief for the uncomfortable symptoms that come with the transition. HUM’s Hormone Balance contains Chaste Berry and Dong Quai which can help with PMS symptoms including mood swings and irritability. However, if you’re looking for something geared a little more specific toward perimenopause/menopause relief, Fan Club’s probiotic formula targets 11 symptoms associated with the transition.
Percentage of participants taking Fan Club and their changes at 4 weeks:
- 90% had a decrease in at least 1 menopausal symptom
- 87% had fewer hot flashes
- 58% had reduced feelings of heart racing
- 62% felt less restless
- 52% had less severe mood swings
- 64% felt less irritable
- 62% felt less exhaustion
- 72% had sex drive improvements
- 49% had less bladder problems
- 49% had less vaginal dryness
- 39% had less join and muscle discomfort
- 64% had less sleep problems
- +slept on average 48 minutes longer
Perimenopause FAQs
How long does perimenopause last?
Perimenopause can last anywhere from a few months to 10 years, with the average being about four years. However, it officially ends when menopause begins (12 months without a period).
Can you still get pregnant during perimenopause?
“Yes, you can still get pregnant during perimenopause,” Agudelo states. “While it’s true that you are not in your peak fertile years, pregnancy is possible in any cycle with ovulation, even when our cycles are not perfect.”
Can I delay menopause or perimenopause symptoms?
While you can’t stop menopause, you may be able to delay its onset by maintaining a healthy lifestyle. Regular exercise, a diet rich in whole foods, and managing stress can all support hormone balance and ease symptoms.
Should I see a doctor for perimenopause symptoms?
If symptoms are affecting your quality of life—like severe mood swings, extreme fatigue, or very heavy periods—it’s a good idea to see a doctor. They can help determine the best treatment options for you.
Can perimenopause make PMS worse?
Many women find that PMS symptoms become more intense or unpredictable during perimenopause. This is due to fluctuating hormone levels. Managing stress, exercising, and tracking your cycle may help alleviate severe symptoms.
The “What is Perimenopause” Takeaway
Perimenopause is a natural yet often challenging phase of a woman’s life. However, this doesn’t mean that you have to suffer through it. While it may feel overwhelming at times, understanding what’s happening in your body can make all the difference. Being able to recognize the symptoms, explore treatment options, and make the appropriate lifestyle adjustments can help navigate this transition with greater ease. Whether it’s seeking support from a healthcare professional, connecting with others going through the same experience, or simply giving yourself grace, you don’t have to go through perimenopause alone. With the proper knowledge and tools, you can take control of your health and embrace this new chapter with confidence.
The post Perimenopause Explained: The Best Supplements and How to Ease Symptoms appeared first on HUM Nutrition Blog.
]]>The post Menopause Does WHAT to Your Sleep?! appeared first on HUM Nutrition Blog.
]]>Of course, getting enough sleep remains an essential piece of your health and wellness, so addressing barriers is important. Understanding how menopause affects sleep can help you prepare and incorporate habits to set yourself up for success.

Menopause and Sleep: The Connection
Sleep issues become more common as women get older. Evidence suggests that approximately 40-50% of perimenopausal women experience sleep disorders and this number can rise to as high as 60% among postmenopausal women.
Why? Menopause comes with a few of its own specific sleep-disrupting characteristics. Many women experience insomnia, hot flashes, and sleep-disordered breathing that makes it difficult to consistently get rest. And understandably so — nobody rests well when they’re overheating, breathing abnormally, or awake into the wee hours of the night for no apparent reason.
As for the underlying causes, we can mostly blame the fluctuating hormones. Menopause is literally the pausing of the menstrual cycle. During this season of life, your ovaries stop producing estrogen and progesterone. These two hormones are heavily involved in your appetite, mood, sex drive, sleep, body temperature regulation, and even your breathing rate — so no wonder all of these things are affected.
Not getting enough sleep is annoying and impacts every aspect of your life beyond bedtime. Adequate sleep is critical for your ability to focus and think clearly, have the energy to engage in your daily activities, for your immune health, and for your long-term wellness.
Now that you know how menopause affects sleep, what can you do about it? Let’s dive into some potential options.
All-Natural Remedies for Better Sleep
The best approach for improving menopausal sleep is to incorporate consistent everyday habits that may help ease symptom severity.
One way to do this is by incorporating natural remedies. While Western medicine and pharmaceuticals certainly have a place in getting through menopause, natural remedies may help alleviate certain symptoms.
Lifestyle Changes to Improve Sleep
Consider what your typical day-to-day routine looks like and identify some areas where improvements could be made to better support your sleep.
Three of the most impactful lifestyle habits include:
- Exercise: A 2022 review found that exercise intervention can be successful in improving insomnia among menopausal women, especially if you have an existing sleep disorder. Consider what types of activity you enjoy doing and carve out time to move intentionally for at least 30-60 minutes most days. Perhaps a combination of swimming, biking, jogging, walking, group fitness, or tennis.
- Stress management: If you’ve ever tried to go to sleep after a stressful event, you know that calming your mind can feel impossible. Incorporating stress management techniques into your regular routine can help. Keep a journal next to your bed, where you can do a “brain dump” at night and release things you’re worried about. Listening to music, stretching and yoga, meditation, and breathing techniques can also be helpful.
- Sleep environment: To promote a good night’s rest, design a sleep-promoting environment. If you’re experiencing hot flashes at night, have layers on your bed that can easily be removed. Wear something breathable that won’t trap sweat. Consider a white noise machine, fan, or blackout curtains if needed.
Dietary Adjustments
Your diet can also be adjusted to better support sleep during menopause. After all, nutrition is a key component of your mental and physical health. Without the proper nutrients, your body has a harder time keeping you healthy.

Add these sleep-promoting foods to your diet:
- Tart cherry juice, which is high in melatonin, a compound produced in your brain as part of your natural circadian rhythm, and may improve sleep time and efficiency
- Walnuts, which are rich in omega-3 fatty acids that may help promote the production of serotonin, a neurotransmitter involved in sleep and mood
- Fatty fish, which are rich in omega-3s as well as vitamin D, which may help promote serotonin production and support normal sleep
- Kiwis, which may promote serotonin production and are also rich in anti-inflammatory antioxidants like vitamin C that may increase sleep duration and reduce sleep disturbances
- Almonds, which provide magnesium, a mineral involved in relaxation that may also support normal sleep
Staying hydrated is also a critical part of your menopause routine. Your body is around 60% water at any given time, and fluid is regularly lost through normal processes like urination, sweating, and other daily maintenance. It’s important to replenish your fluids for proper temperature regulation and immune function.
If you struggle to stay hydrated, consider these tips:
- Fill a reusable water bottle in the morning to take with you
- If you get bored of plain water, add fresh lemon or cucumber slices for natural flavoring, or try unsweetened seltzer water
- Start your day with a glass of water versus drinking a bunch at night, as the latter may disrupt your sleep due to trips to the bathroom
Herbal Supplements
Many women find that adding herbal supplements to their sleep routine can help them achieve better rest at night. Some of these include:
- Valerian root, which contains an active compound called valerenic acid, which is responsible for its sedative effects
- Lavender, a flowering plant in the mint family that may have anti-anxiety, sedative, and brain-protective properties
- Passionflower, which offers anti-anxiety, sedative, and mood-supportive benefits
- Turmeric, an Indian spice with the bioactive component curcumin, which offers anti-inflammatory and antioxidant effects and supports brain health
Note that herbal supplements aren’t for everyone and can interact with certain medications and other supplements. Speak with your healthcare provider before adding these to your sleep regimen.
Calming Nighttime Drink Recipes
Sometimes, starting your nighttime routine with a warm, soothing beverage can help set you up for better sleep success. Here are three recipes that are not only simple and tasty but also contain ingredients that may help prepare your mind and body for rest.

Herbal Sleep Tea
Ingredients
- 1 tsp dried passionflower
- 1 tsp dried lemon balm
- 1 tsp dried chamomile
- Boiling water
- Optional: honey or other sweetening agent
Preparation
Combine your dried herbs together in a tea ball or reusable tea bag and place it in your mug. Add boiling water to fill your mug and allow your tea to steep for 3-5 minutes or per your liking. Remove your tea bag from the water and gently mix in your desired sweetening. Serve.
Golden Milk
Ingredients
- 1 cup unsweetened plain soy milk
- ½ tsp ground ginger
- ½ tsp ground turmeric
- ½ tsp ground cinnamon
- 1 Tbsp unsweetened cashew butter
- Pinch of black pepper (to help boost the absorption of curcumin from the turmeric)
- Optional: sweetener of choice
Preparation
Combine all of your ingredients in a saucepan and whisk them together while heating over medium heat. Continue to stir gently and heat for 3-5 minutes until well combined and warmed throughout. Serve.
Lavender Chamomile Infusion
Ingredients
- 1 tsp dried chamomile
- ½ tsp dried lavender
- Optional: ½ tsp dried mint, sweetening agent
- Boiling water
Preparation
Combine your dried herbs (and optional mint) in a tea ball or reusable tea bag and place it into your mug. Fill your mug with boiling water. Allow herbs to steep for 3-5 minutes before removing. Add an optional sweetening agent and serve.
Incorporating HUM Products
In addition to products designed to help support your overall health and wellness, HUM also makes some that may be particularly beneficial for menopausal support, like:
Berberine is a plant compound found in things like European barberry and goldenseal. Designed to be taken daily with food, our berberine capsules help support the body’s glucose and fat metabolism for healthy glucose and cholesterol levels*. They contain BioPerine®, a patented piperine derived from black pepper that helps nutrient absorption*. Additionally, berberine supports beneficial bacteria and promotes a healthy gut microbiome.
This daily capsule is an estrogen-free, non-hormonal, clinically studied probiotic formula that addresses 11 symptoms of perimenopause and menopause. It features ingredients like Siberian rhubarb extract to reduce the severity of hot flashes, night sweats, vaginal dryness, fatigue, and irritability, patented probiotics to support the gut-brain axis and mood, and grape seed extract for stress support.
Be sure to consult with your healthcare professional before adding any new supplements to your routine, to ensure that they are safe and appropriate for you.
Rest Easier During Menopause
Sleep is an essential element to your quality of life and everyday health. Unfortunately, getting enough of it on a consistent basis is easier said than done during menopause. When you’re experiencing side effects of such dramatic hormonal changes, like hot flashes, night sweats, and insomnia, it’s difficult to find restful sleep.
The good news is that there are everyday habits and dietary changes that may be helpful. Explore natural remedies and calming drinks to see what helps you. Consider adding a HUM product like Best of Berberine or Fan Club to help support your best health and rejuvenation during menopause.
to help support your best health and rejuvenation during menopause.
The post Menopause Does WHAT to Your Sleep?! appeared first on HUM Nutrition Blog.
]]>The post 4 Pelvic Floor Exercises To Try (Because It’s Not Just Kegels) appeared first on HUM Nutrition Blog.
]]>When exercising, many of us focus on the main groups, such as the legs, arms, glutes, and core—but these aren’t the only muscles that need movement and training to remain resilient, flexible, and strong. Although you can’t see them, the pelvic floor muscles that reside deep in the pelvis can have a lasting impact on our overall health and well-being because they are connected to many important bodily functions.
“The pelvic floor is made up of a group of muscles that forms a hammock at the base of the pelvis,” says Madelaine Golec, a pelvic health physiotherapist at ECO Physiotherapy. She explains that the pelvic floor is responsible for supporting the pelvic organs (think: the bladder, uterus or prostate, and rectum). “These muscles help to control the flow of urine and feces, are involved in sexual function, keep circulation moving through the pelvis, and part of our core that supports the movement of the hips, back, and pelvis,” she adds.
Pelvic floor exercises date back as far as Ancient Greece and Ancient Rome. However, topics surrounding the pelvic floor (including exercises) have remained relatively taboo—that is, until recently. These days, the health and wellness world is experiencing a pelvic floor revolution, with ever-growing awareness of the importance of pelvic floor muscles in overall well-being. “Studies have shown that pelvic floor dysfunction (problems with muscles, ligaments, and nerves) can lead to a range of issues such as incontinence, pelvic organ prolapse, sexual dysfunction, and pain,” Golec explains. She adds that these symptoms were originally thought to be a normal part of aging, childbirth, or injury, and you “just had to cope with it” or get surgery. But now, many medical professionals have turned to pelvic floor exercises for prevention and treatment alike.
What Is Pelvic Floor Therapy?
Pelvic floor therapy includes exercises that can strengthen and improve the overall health of the pelvic floor. It’s essentially physical therapy for the muscles, ligaments, and nerves of the pelvic floor. When we think of pelvic floor exercises, many of us think about Kegels, which became popular in the 1950s by Dr. Arnold Kegel (hence the name). However, to strengthen your pelvic floor as best you can, you’ll want to go beyond Kegel exercises alone.
“Pelvic floor therapy is different from Kegel exercises because Kegels are just a specific type of exercise that is designed to strengthen the pelvic floor muscles,” says Golec. While Kegels are important and among the best pelvic floor exercises, others may be recommended.
In addition to Kegels, Golec says pelvic floor therapy focuses on treatments like:
- Pelvic floor relaxation
- Exercises to improve muscle strength and coordination (not just of the pelvic floor muscles, but all the muscles around the pelvis and back, too)
- Manual therapy to improve mobility and flexibility
- Education about body mechanics
- Breathing and lifestyle factors that can affect pelvic floor health

Signs of a Weak Pelvic Floor
While pelvic floor exercises are beneficial for everyone, those with weak pelvic floors can experience a transformation through strengthening and building resilience in the deep core.
Some of the most common signs of a weak pelvic floor include:
- Incontinence, aka leakage of urine or feces
- Difficulty with bowel movements or urination
- Bulging, heaviness, or pressure in the pelvic area
- Pelvic pain
- Difficulty with sexual function, including pain during sex or difficulty achieving orgasm
- Low back pain
- SI joint pain and/or hip pain
- Tight pelvic floor muscles that are difficult to relax
Benefits of Pelvic Floor Exercises
A weak pelvic floor is a reason in and of itself to try pelvic floor exercises, especially since consistent exercise can make a difference in the symptoms associated with it and therefore offer relief. But according to Golec, everyone can benefit from pelvic floor exercises—no matter your age or gender—and even if you already have a healthy pelvic floor. “As with any other muscles in the body, we want to have strong and flexible muscles for overall day-to-day function, and we often don’t think to include our pelvic floor,” she explains.
Pelvic floor exercises are particularly important for those who are pregnant or postpartum, “as these muscles can be weakened by the changes in the body that occur during pregnancy and childbirth,” says Golec. Being proactive with pelvic floor exercise is also helpful during perimenopause and menopause since hormones change and can affect the hammock of muscles.
P.S. Seeking relief from menopause symptoms like hot flashes, vaginal dryness, and mood swings? Check out HUM’s Fan Club.
But what about men? “For men, it is important to start pelvic floor exercises before and after prostate surgery, especially the removal of the prostate,” Golec adds. According to Jennifer Self Spencer, PT, DPT, CLT, OCS, a pelvic floor physical therapist at Magic City Physical Therapy, “Men can also experience bowel and bladder symptoms, erectile dysfunction, pelvic and genital pain, and hip, groin, abdominal, and low back pain that can be attributed to pelvic floor dysfunction,” she shares, which makes strengthening the pelvic floor all the more important for men, too.
If you experience any of the signs of a weak pelvic floor—even minimally—Spencer recommends seeing a pelvic floor therapist. “Pelvic floor symptoms often get worse over time, so it is best to get [them] under control sooner rather than later,” she explains, adding that painful conditions are easier to treat in the acute phase (versus waiting until it transforms into chronic pain).
How to Strengthen the Pelvic Floor
Strengthening the pelvic floor through exercise can be done with the help of a professional, as well as at home for preventative measures. Below, experts share four of the best ways to strengthen the pelvic floor.
1. Kegel Exercises
According to Golec, you can’t go wrong with a classic Kegel exercise. “To do Kegel exercises, pretend to stop the flow of urine,” she explains. Note: You don’t want to practice this while actually peeing; this is simply a good way to visualize what your body needs to do. “Try to squeeze and lift the muscles for a count of three, then relax for a count of three,” she continues. From there, Golec recommends adding in some breathwork and coordinating the muscles with breathing. “Try to relax the pelvic floor on the inhale and ‘hold your pee’ on the exhale, working your way up to 10 reps.”
Ladies: Take a look at HUM’s Private Party, a probiotic that supports vaginal pH balance. It also includes cranberry PACs to promote healthy urinary tract function.
2. Diaphragmatic Breathing
“The diaphragm moves in direct coordination with your pelvic floor,” says Joelle Spadaccini, a certified prenatal/postpartum corrective exercise specialist and certified Pilates instructor at Niche Pilates Studio. She adds that the diaphragm expands on an inhale and contracts on an exhale. “Taking deep breaths in and out will work on strengthening the coordination of the pelvic floor,” she explains. Through this process, the pelvic floor should relax, contract, and lift—thus building strength, flexibility, and resilience.

3. Squat With Pelvic Floor Contraction Breath
Spadaccini also recommends adding a functional movement to Kegels and diaphragmatic breathing to train the body to properly function. “Start with your feet hip-width apart and inhale as you sit back and down into a squat while relaxing the pelvic floor,” she explains. From there, begin to stand up and exhale to contract your pelvic floor until you are back in a full standing position. “Once you are back at the top, attempt to hold the contraction of the pelvic floor for 10 seconds.” Then try to completely relax the pelvic floor again while sitting back and down into the next squat. Spadaccini says this exercise takes a lot of focus and coordination from the entire body but, over time and with practice, it can happen naturally when you bend down to pick something up off the floor.
4. Bridges
Bridge exercises are also among the best pelvic floor exercises to try at home. “To do a bridge, lie on your back with your knees bent and your feet flat on the floor,” Golec instructs. “Tighten your pelvic floor muscles and lift your hips off the floor, holding the position for a count of three before lowering back down,” she adds. For an effective circuit, Golec recommends starting with at least 10 reps.
In addition to these exercises, there are a few tips and tricks you can follow for a healthy and strong pelvic floor. “Drink plenty of water and limit bladder irritants like soda, coffee, tea, seltzers, and alcohol,” Spencer advises. She also recommends getting plenty of fiber during the day, noting that adults generally need around 25 to 35 grams of fiber daily. Another way you can support the pelvic floor is by limiting straining while having a bowel movement. Spencer also recommends utilizing a toilet stool and deep breathing.
The Takeaway
Although we can’t see these muscles, the pelvic floor plays a key role in several bodily functions and our overall well-being—so it’s important not to ignore it. And while those with weak pelvic floors are advised to work with a pelvic floor therapist and practice the exercises above, everyone can benefit from Kegels, breathwork, bridges, and other pelvic floor exercises.
The post 4 Pelvic Floor Exercises To Try (Because It’s Not Just Kegels) appeared first on HUM Nutrition Blog.
]]>The post This Ancient Herb Is Your Ally Against Cramps appeared first on HUM Nutrition Blog.
]]>Dong quai is an herb that’s root has been used in Traditional Chinese Medicine for over one thousand years. It is celebrated for its ability to regulate hormones and aid in menstrual-related issues. In addition to its use for reproductive health, it is also used for respiratory, digestive, and immune support. Less common, but still notable, you may be familiar with it as a culinary herb, sometimes making its way onto the dining table via salads or roasts. It is also a common ingredient in various liqueurs and liquor and is popular in artisanal bitters.
As an herbalist, I’ve worked a lot with this plant. I’ve seen first-hand the benefits of dong quai related to the reproductive system. Below, I’ll explore how it acts as an ally from the literal start to finish of the menstrual cycle.
What is Dong Quai?
The scientific name for Dong Quai is Angelica sinensis. It is native to Japan, Korea, and the mountains of China, particularly the Shanxi and Gansu provinces. Its white blooms open in the summer, and roots, seeds, and leaves are all used for medicinal purposes. Herbalists often use it alongside other herbs in formulations to aid in symptoms associated with menopause and menstruation. Dong quai root is particularly popular.
Dong Quai Benefits
From menstrual regulation to menopause, dong quai is a go-to for myriad women’s health concerns. One of its most well-known mechanisms is hormone regulation. This makes it a natural choice for symptoms of PMS, menopause, and beyond. These are some of the top dong quai benefits:
Reduces Hot Flashes
During menopause, there is a steep decrease in both estrogen and progesterone. The change in hormones can lead to many symptoms, including hot flashes. Estrogen and progesterone also directly affect the hormone serotonin, which can play a role in decreasing hot flashes. That’s where dong quai comes in. Dong quai can help alleviate hot flashes by regulating hormones due to its potential serotonergic (a.k.a. it affects serotonin) activity. In a binding assay (an analytic procedure measuring the interaction between two molecules) involving the 5-HT7 serotonin receptor, dong quai exhibited serotonin-like activity. Because dong quai is capable of increasing serotonergic activity, it may help to improve symptoms of hot flashes, even when the body isn’t producing enough estrogen or progesterone to regulate serotonin on its own. (Psst: Siberian rhubarb root is another powerful herb for relieving hot flashes. That’s why we put it in our perimenopause and menopause supplement, Fan Club.)
Alleviates PMS Symptoms

Dong quai also may help relieve a number of symptoms associated with PMS, including painful cramping. It contains a bioactive constituent called Z-ligustilide, which may help reduce cramping by minimizing uterine contractions and helping with circulation. It is at least partially responsible for dong quai’s antispasmodic and anti-inflammatory attributes. Ferulic acid is another key active compound found in dong quai. It can act as an analgesic, or pain reliever, and may contribute to dong quai’s cramp-fighting abilities. Another bonus? The same hormone-regulating effect dong quai has on menopause symptoms can also help diminish unwanted symptoms associated with PMS, such as mood swings and bloating, since hormone fluctuations can be responsible for both of these.
Stimulates Blood Flow
There’s been a traditional association between dong quai and blood itself. It’s not surprising then, that it has been used to stimulate the arrival of a delayed period. It can act as an anticoagulant and, as discussed earlier, promotes blood circulation. It is thought that the polysaccharides in dong quai are a major contributing factor to replenishing blood and moving it out of a stagnant state. In this way, dong quai may help regulate the menstrual cycle and keep things flowing, so to speak.
Who Should Take Dong Quai?
Dong quai can be a wonderful choice for folks who struggle with irregular or painful periods, or those going through menopause. As with any new supplement, it’s important to discuss with your doctor before adding dog quai to your routine. If you are pregnant or breastfeeding, should avoid the plant given it’s effect on the reproductive system. It is also a good idea to skip this one if you are on anticoagulants or antiplatelets, as it can potentially heighten their effect. If you are prone to particularly heavy periods, dong quai may not be the best choice for you.
Dong Quai Side Effects
Minor side effects to be aware of include photosensitivity and gastrointestinal issues. As always, listen to your body and consult a healthcare professional if anything seems amiss. Furthermore, if foraging is your thing, don’t try and collect this plant yourself. Not only is it easy to mistake dong quai with poisonous plants, but its roots are toxic until you’ve dried them. It’s best to take dong quai in the form of a high-quality supplement.
What Should I Look for in a Supplement?

Now that you’re on the road to relief from menstrual mayhem, it’s important to make sure you’re getting the most out of your dong quai supplement that you can. In Traditional Chinese Medicine, dong quai is almost always taken in conjunction with other herbs for a synergistic effect. Capsules are one of the more convenient and reliable ways to ensure that the dosage and quality is consistent. HUM’s Moody Bird contains the recommended 150 milligrams of dong quai powder and 300 milligrams of chasteberry in a vegan capsule. Moody Bird not only helps with the physical symptoms of PMS, but also works on the emotional side, bringing some freedom from mood swings and irritability that so many experience in the early days of our cycle.
The Takeaway
It’s clear to see why dong quai has been a mainstay in herbal medicine for the past millennium. Its action on the reproductive system and rich healing history are equally compelling facets of this ancient plant. Like so many other plants with complex chemistry, we will most likely continue to uncover the mysteries of its various healing mechanisms. In the meantime, enjoy the relief, regulation, and relaxation that this tried and true herbal ally can bring to your life and cycle.
The post This Ancient Herb Is Your Ally Against Cramps appeared first on HUM Nutrition Blog.
]]>The post The Results Are In: HUM’s Fan Club Is Clinically-Proven to Decrease Menopause Symptoms in 90% of Users appeared first on HUM Nutrition Blog.
]]>The impact that menopause can have on daily life is often overlooked and women have few options to help them manage perimenopause and menopause symptoms.
To give women a natural, estrogen-free solution to help reduce 11 common symptoms of menopause and perimenopause, HUM created Fan Club. Fan Club contains three key ingredients that have individually been studied to support symptoms of menopause like hot flashes, night sweats, sleeplessness, mood swings, heart racing, and fatigue.
Fan Club’s standout ingredients are:
- Siberian rhubarb root extract
- The probiotic Lactobacillus plantarum DR7
- Grape seed extract
Together, these ingredients are a powerful tool for managing symptoms and helping women regain control of their lives during perimenopause and menopause. But just how powerful are they?
We put Fan Club to the test. Or rather, took it to the lab to get clinically-backed results.
“The ingredients we use in Fan Club have really robust evidence to support their effect of improving many menopause symptoms,” says Jennifer Martin-Biggers, PhD, MS, RDN, the VP of scientific affairs and education at HUM Nutrition. “It was important for us to support users of Fan Club with additional science to show how efficacious this can be to help relieve a variety of symptoms.”
Find out how well it performed under the microscope.
How the Study Worked
To ensure no bias in our study, we worked with an independent, third-party clinical research lab in California to perform a randomized, double-blind, placebo-controlled clinical study. The lab enrolled over 100 women experiencing menopause symptoms to participate.
The research lab adhered to clinical research ethical and legal requirements. To ensure that a clinical study is conducted ethically, an independent ethics committee, called an Institutional Review Board (IRB), reviewed the study plans to make sure it was safe and designed according to research standards.
The final study included 111 perimenopausal women with mild, moderate, or severe symptoms.
The participants were split up into two groups, either the experimental group that received Fan Club, or the control group that was given a placebo. Neither the study administrators nor the participants knew which group they were in.
Both groups were instructed to take the active or placebo supplement once daily for 8 weeks. They were given surveys to assess their symptoms at baseline, and then 30 and 60 days after beginning the supplement.
Questions in the survey were designed to assess changes in menopause symptoms including hot flash and night sweat frequency and severity of 11 total menopause symptoms, as well as hours slept.
Result Highlights
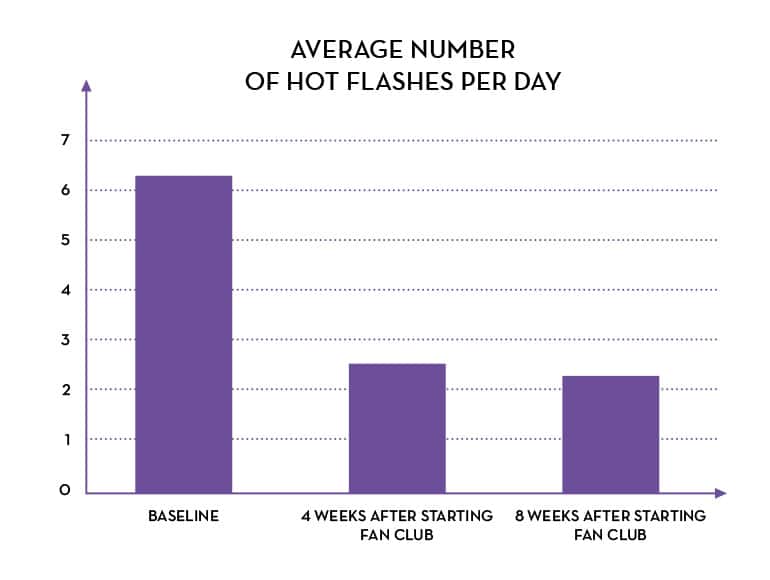
The majority of participants started to see results between three to four weeks. After four weeks of taking Fan Club once per day, the experimental group had significant improvements in symptoms.
- 90% of participants witnessed positive results
- 87% of participants had fewer hot flashes
- The number of hot flashes participants had decreased by 60%
- Participants had a 40% decrease in total symptom score
- 64% of participants had fewer sleep problems, and as a bonus, they slept on average 48 minutes longer
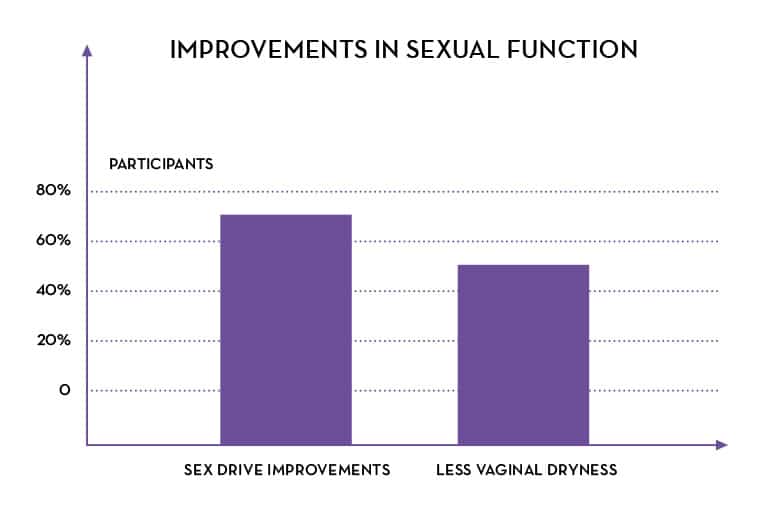
- 72% of participants had sex drive improvements
- 49% of participants had less vaginal dryness
- 64% of participants felt less irritable
Statistical analysis showed these results to be statistically significantly decreased among participants in the Fan Club group, compared to those in the placebo group. An evaluation of statistical significance is performed with study data to help quantify if a result is due to chance or actually a result of efficacy or performance. The statistical significance of the Fan Club study indicates the formula is clinically efficacious.
Women also reported significant decreases in the frequency and severity of other menopause symptoms including:
- Heart racing
- Joint and muscle discomfort
- Restlessness
- Mood swings
- Bladder problems
- Exhaustion
“The most impressive result is that this study tells us Fan Club starts to have a profound effect alleviating symptoms as soon as 4 weeks after taking it, and these results persist,” explains Dr. Martin-Biggers.
Throughout the course of the eight-week study, there were no adverse events reported related to Fan Club.
What Users Had to Say
While the numbers speak for themselves, we thought we’d let our trial participants do the talking, too, because their love for Fan Club is unmatched. Here’s what a few had to say about their experience after 8 weeks of taking Fan Club.

“I absolutely LOVE this product ‘cause it actually works! It has literally given my life back to me! I cannot THANK YOU enough!!!”
“I hope at the end of the test that we’re able to buy this because I’m crying happy tears just writing about this.”
“I feel very different to the way I felt 2 months ago. I have only experienced one hot flash in the past month and several other beneficial changes.”
“I no longer have hot flashes, sweating a lot, or sleeplessness. My mood and anxiety have ceased as well! My overall well-being has improved drastically!”
“I’ve tried so many different things and nothing has worked since this.”
Join the Fan Club

We’re so happy at the results of the randomized, double-blind, placebo-controlled clinical study of Fan Club, but even more, encouraged by the meaningful impact Fan Club can have on the lives of women going through perimenopause and menopause.
“I am thrilled with the results but not surprised by them as the ingredients we used have great science supporting their effectiveness,” says Dr. Martin-Biggers.
Ready to join the Fan Club with us? (We thought so!) If you’re dealing with menopausal symptoms, Fan Club is the perfect supplement to add to your daily routine, says Dr. Martin-Biggers.
The post The Results Are In: HUM’s Fan Club Is Clinically-Proven to Decrease Menopause Symptoms in 90% of Users appeared first on HUM Nutrition Blog.
]]>The post 8 Causes that May Be At the Root of Your Hair Loss appeared first on HUM Nutrition Blog.
]]>Whether you’ve spent your life trying to style thick, unruly strands into submission or add volume to limp locks, you’ve probably thought of your hair as “problem hair” at some point. But if you’ve been noticing more hair in your shower drain lately or your hair is starting to thin, that term has taken on new meaning—and new concern. What’s causing this sudden bout of hair loss? And, more importantly, can you stop it?
The first thing you should know is that you’re not alone. Experts estimate that more than 50 percent of women will experience hair loss at some point in their lives, with around 30 million women (or about a third of that number) suffering from female pattern hair loss. But that’s just one potential cause of your hair woes—and you need to figure out what’s actually going on to effectively treat and ideally reverse this problem.
So, how much hair loss is normal?
Let’s get right to it: According to the American Academy of Dermatology (AAD), it is normal to shed anywhere from 50 to 100 strands of hair per day. The Cleveland Clinic adds that this number may go up slightly if you wash your hair only once or twice a week, especially if you have long hair, due to a buildup of hair that’s on its way out. This is all part of your hair’s normal life cycle: anagen (active growth), catagen (transition), and telogen (resting and shedding). This cycle takes anywhere from two to six years, and you usually don’t notice it since your follicles are all at various stages of growing and shedding.
Things are decidedly not normal, however, “if you are experiencing hair shedding of greater than 125 strands a day or if you have observed bald spots on your scalp or a widening of your hairline,” says Michele Green, MD, a dermatologist at Lenox Hill Hospital in New York City. That’s when it’s time to take a closer look at your hair health.
Hair loss vs. hair shedding: What’s the difference?

The AAD states that hair loss occurs when something stops the hair from growing. True hair loss (aka anagen effluvium), when not resulting from an outside factor like chemotherapy or harsh hairstyling chemicals, is often the result of genetics, says trichologist Penny James, owner of the Penny James Salon in New York City. James notes that with female pattern baldness, or androgenic alopecia, women will notice thinning near the temples and the crown area—something you may have noticed in your female relatives. If, however, you’re noticing small round patches without hair on your scalp, that’s likely the result of an autoimmune disorder (alopecia areata) that attacks hair follicles. While subsequent hair loss can be halted and there are treatments that can help, whether or not the condition is reversible depends on its cause.
On the other hand, excessive hair shedding (telogen effluvium) occurs “when the hair growth cycle has been interrupted and the hair has been pushed prematurely into the telogen stage—the falling-out stage,” James explains. This can be caused by a variety of factors including diet, stress, hormonal changes, and styling. James notes that the shedding will usually be all over the head, as opposed to localized patches, but it may be more noticeable in already-thinner areas. The good news is that in most cases, once you address the underlying issues, you won’t necessarily have lasting problems.
The causes of hair loss
So, what’s at the root of your problems? It’s essential to figure that out so you can proceed with the correct course of treatment, whether it’s a relatively simple fix you can handle yourself or something that will require more aggressive intervention. Of course, it’s always a good idea to consult a professional, who can make sure you’re on the right track and evaluate your overall health, but the following common causes can help you narrow things down.
Menopause
Yep, the same hormonal changes that can cause hot flashes, night sweats, weight gain, and other delightful issues can also lead to hair loss. “During menopause, levels of estrogen are decreased,” explains Dr. Green. “The decrease in estrogen can lead to heightened androgen sensitivity and, in turn, cause weakening and shrinkage of the hair follicles.” Treatments for menopause-related hair loss can range from oral medication and hormone replacement therapy to topical Minoxidil treatments and platelet-rich plasma (PRP). (More on PRP therapy below.)
Stress
Not to stress you out further, but stress itself may actually be causing your hair to fall out. “Stress is a huge problem with hair loss,” says James. “I would say 90 percent of my clients are suffering from acute stress these days.” She explains that when you are stressed, the hormone cortisol wreaks havoc on your body, potentially affecting your thyroid and adrenal glands, aggravating your scalp, and even causing eczema, psoriasis, seborrheic dermatitis.
At the most basic level, that hormone surge, says Dr. Green, can disrupt the hair growth cycle, causing hair to go into a longer period of rest and stop growing. It can take six weeks to six months after a stressful event for hair loss to occur. While most people’s hair will rebound on its own once this cycle of stress and loss has passed, Dr. Green notes that certain types of stress-related hair loss can be permanent if not treated early.
Sickness
Your fever may have broken long ago and that illness may now be a distant memory for you…but your body still remembers. Any major health event, especially one that comes with a high fever, can push more hair than usual into the shedding phase, but you won’t experience this shedding until a few months later. While this side effect may last for six to nine months, the good news is that it should eventually stop on its own.
In case you were wondering, yes, this has been yet another unexpected side effect of COVID-19. Aside from the plethora of anecdotal evidence, one study from China published in The Lancet found that 22 percent of those hospitalized with COVID were still reporting hair loss six months after they were discharged. While this can happen with any major illness, COVID can hit you with a double dose of physical and emotional stress.
Nutrient deficiencies
As they say, you are what you eat—and if you’re not getting the proper nutrients, your hair will reflect those deficiencies. “Poor nutrition can cause malabsorption and inflammation in the body, which can disrupt the growth cycle of the hair,” says Dr. Green. “Inflammation does not allow the cells to repair completely, and that cell damage results in hair loss.” A nutrient-dense diet, on the other hand, can aid in proper absorption, cellular turnover, and hormonal balance and lead to longer, stronger, healthier hair.
First, make sure you’re getting a proper amount of amino acids and proteins. If you’re low on protein, James says, you might be anemic, which can drive down your iron and cause hair shedding. Beyond that, she says to look into vitamins A, C, D, and E, as well as B complex and zinc, which are important for healthy follicles and hair growth. If your diet has certain restrictions or you’re trying to lose weight, you should pay special attention to this. (Side note: Significant weight loss—think 20-plus pounds—can also be a shock to your system and cause hair loss.)
Hormonal issues
A decrease in estrogen during menopause isn’t the only hormonal issue that can affect your hair. Both hypothyroidism and hyperthyroidism can result in hair loss, and if either is autoimmune-related, it can result in the previously discussed alopecia areata. Polycystic ovary syndrome (PCOS) can also be the culprit. Higher-than-normal levels of male hormones, or androgens, in women with PCOS can “cause the hair follicles to thin out and shrink over time, leading to female pattern baldness,” says Dr. Green. In both cases, getting your hormones on track (albeit in different ways) can help with all of your symptoms, including hair loss.
Pregnancy
Your hair will never look as luxurious as when you’re pregnant…or as lackluster as in the weeks after giving birth. This excessive shedding results from falling estrogen levels, according to the AAD, and generally peaks about four months after giving birth. While it can be disconcerting to see more hair in your brush or thin patches on your scalp, your hair should return to normal within 12 months. Still, make sure you’re getting proper nutrients and keep an eye on your stress levels so that this pregnancy-specific issue doesn’t spiral into another one.
“Pulling” hairstyles
Sometimes, the things we do to make our hair look amazing can completely backfire. That’s the case with certain hairstyles, including tight buns and ponytails, as well as tight braids, hair extensions, and weaves. The pulling inherent in these styles can cause a type of hair loss known as traction alopecia—which, if not dealt with, can result in permanent hair loss. If you notice broken hairs around your hairline, a receding hairline, or patchy loss, it might be time to loosen up your hairstyle for a while and allow hair to heal and recover.
Overstyling
Similarly, repeated harsh chemical treatments—from relaxers to perms—can be problematic and, in extreme cases, cause scarring of the scalp, which would impede hair growth. On the other hand, over-styling with hot tools (especially if they’re not used correctly), dyeing hair too frequently, and aggressive brushing can make strands brittle and cause them to break more easily. While these latter issues do not result in true hair loss, your broken strands can exacerbate thinning and cause hair to look less than fabulous.
What can you do to prevent hair loss and improve hair growth?

As mentioned earlier, your path forward really depends on what’s causing your hair loss or shedding. Hormonal issues, for example, may require medication to treat the larger issue; hair loss is simply a side effect. The same goes for hereditary hair loss that may be halted and helped with oral or topical medication or something like PRP (platelet-rich plasma). With this treatment, explains Dr. Green, a doctor injects concentrated blood plasma (created with your own blood but containing up to five times more platelets than it normally does) into your scalp. This can improve cell reproduction and blood vessel formation while also healing and stimulating hair follicles.
While a professional can help you determine the best course of action, you can also do your part at home to stem the tide of shedding hair. Here are a few things everyone can try:
- Keep stress in check. “The first step is to know you are stressed,” says James. “Then take action: Meditate. Take a walk outside. Turn off the phone. If you need to, seek professional guidance.”
- Make sure you’re getting the right vitamins and minerals. In addition to incorporating more of the good stuff in your meals, supplements can also work wonders. Zinc and biotin (one of the B complex vitamins) are two dermatologist and trichologist favorites since they help with follicle health and hair growth and strength, respectively. HUM’s Hair Sweet Hair contains both of these, as well as folic acid, fo-ti, B12, and PABA. (Bonus: These yummy gummies are also vegan.)
- Be kind to hair when styling it. “Our hair is a fiber made of protein and can only take so much heat before it burns and breaks off,” says James. “The key is to take organized sections when using a heated tool and not have the heat setting on too high.” If hair is fragile, she also recommends staying away from brushes with metal centers and plastic bristles and using wooden brushes with boar bristles instead.
- Keep hair hydrated. Your choice of product will depend on your specific type of hair, but making sure that hair isn’t overly dry is key to maintaining cuticle health, says James. While B vitamins are a boon when consumed, there are no scientific studies that prove biotin is as effective when applied topically. That said, hair experts swear by certain biotin-infused shampoos and conditioners for keeping hair nourished and follicles healthy.
Now take a deep breath. If you are experiencing any form of hair loss, it can feel devastating, but you have options. Finding a targeted treatment that’s right for you can change everything—and lead to the healthiest, fullest, most gorgeous hair you’ve ever had.
The post 8 Causes that May Be At the Root of Your Hair Loss appeared first on HUM Nutrition Blog.
]]>The post Your Secret Ingredient Against Hot Flashes? Siberian Rhubarb Root. appeared first on HUM Nutrition Blog.
]]>What is Siberian rhubarb root?
Siberian rhubarb, also known as rhapontic rhubarb, is an extract from the roots of a plant called Rheum rhaponticum. Although they sound similar, Siberian rhubarb root is not the same species as garden rhubarb, a vegetable commonly used for food.
This plant has been around for centuries and originates back to Northern and Central Asia. However, it gained popularity during the 90s when it became commercially available in Germany for the treatment of hot flashes.
Today, Siberian rhubarb root can be found in dietary supplement form, like HUM’s Fan Club, to address menopause symptoms.
Benefits of Siberian rhubarb for menopause
Siberian rhubarb root in its standardized form, ERr 731 , has been shown in clinical studies to help ease the severity of menopause symptoms.
, has been shown in clinical studies to help ease the severity of menopause symptoms.

Hot flashes
During menopause, estrogen levels fluctuate and trend downwards. Many processes throughout the body rely on balanced estrogen levels. One example is thermoregulation, the process that regulates body temperature. Thermoregulation relies on estrogen receptors in the brain to function normally. Naturally, when estrogen levels decline, it can lead to dysregulation of body temperature and you guessed it, hot flashes.
That’s where Siberian rhubarb root comes in. It works by activating the same estrogen receptors that influence body temperature. As a result, it can help reduce how often hot flashes occur. There are currently four clinical studies supporting its ability to provide relief from hot flashes.
One study evaluated the effect of 4 mg of Siberian rhubarb root in 100 perimenopausal women with complaints of hot flashes. After 28 days, participants felt less moderate to severe hot flashes occurred.
A similar trial further confirmed the reductive effect of Siberian rhubarb root on hot flashes over a longer period of time (12 weeks). It may also help with night sweats, which are essentially hot flashes at night.
Other menopause symptoms
While hot flashes are one of the most common symptoms of menopause, many women experience other symptoms, too. It brings about an array of uncomfortable bodily changes. Nevertheless, Siberian rhubarb can help ease those too.
An open observational study found that 4 mg of dried ERr 731 resulted in significant improvement of menopausal symptoms according to the Menopause Rating Scale (MRS). Impressively, researchers saw a decrease from 14.5 points at baseline to 6.5 points after six months of taking the extract daily. In addition to fewer hot flashes, participants also reported a decrease in irritability, sleep problems, and physical/mental exhaustion.
resulted in significant improvement of menopausal symptoms according to the Menopause Rating Scale (MRS). Impressively, researchers saw a decrease from 14.5 points at baseline to 6.5 points after six months of taking the extract daily. In addition to fewer hot flashes, participants also reported a decrease in irritability, sleep problems, and physical/mental exhaustion.
Also, a clinical study evaluating perimenopausal women taking the extract daily reported improvements in mood, according to the Hamilton Anxiety Scale, and overall quality of life.
Who should try Siberian rhubarb?
Based on the present research, Siberian rhubarb root is beneficial for perimenopausal and menopausal women experiencing daily symptoms. ERr 731 can help women dealing with:
can help women dealing with:
- Hot flashes
- Irritability
- Mood swings
- Sleep problems
- Exhaustion
- Vaginal dryness
- Joint and muscle discomfort
In addition, it delivers results fairly quickly. Most people taking the extract begin feeling improvements as soon as 28 days.
Moreover, ERr 731 boasts an impressive safety profile with no adverse events reported in the relevant body of literature.
boasts an impressive safety profile with no adverse events reported in the relevant body of literature.
Its long-term safety and effectiveness has been evaluated at 48 and 96 weeks. Researchers concluded that the extract is both safe and effective in the long-term use for menopausal discomforts.
However, women undergoing hormone-replacement therapy (HRT), a common treatment for menopause symptoms, or who are taking other prescription medications should still consult with their doctor before adding Siberian rhubarb root to their routine.
What to look for in a Siberian rhubarb supplement

Siberian rhubarb root’s bioactive compounds: rhapontigenin and desoxyrhapontigenin, and their metabolites resveratrol and piceatannol are responsible for its benefits. The patented ERr 731 , delivers a standardized version of the extract that delivers the proven ratio of the bioactive compounds. In other words, it has the ratio that the clinical studies (and results) are based on.
, delivers a standardized version of the extract that delivers the proven ratio of the bioactive compounds. In other words, it has the ratio that the clinical studies (and results) are based on.
For best results, it’s also very important to make sure you are getting the right amount of ERr 731 . The clinically effective dosage for Siberian rhubarb root is 4 mg daily.
. The clinically effective dosage for Siberian rhubarb root is 4 mg daily.
Final thoughts
Menopause can be a challenging time for the mind and body. Clinically studied Siberian rhubarb root has proven to help make life easier while transitioning through menopause. Unlike other approaches for menopause symptoms, this extract can deliver significant relief without unwanted side effects. HUM Nutrition’s Fan Club supplement delivers 4 mg of Siberian rhubarb root.
The post Your Secret Ingredient Against Hot Flashes? Siberian Rhubarb Root. appeared first on HUM Nutrition Blog.
]]>The post 7 Ways to Manage Menopause Weight Gain appeared first on HUM Nutrition Blog.
]]>Depending on whether you’re in perimenopause, have reached menopause, or are post-menopausal, you could be experiencing any combination of symptoms: vacillating between chills and night sweats, thinning hair, dry skin, vaginal dryness, low libido, and even mental health-related symptoms such as anxiety, depression, and insomnia. Another common signifier of the menopausal period is the overall slowing of your metabolism, and in some cases, menopause weight gain. Blame your hormones on what some call a “menopause belly,” but know that every hormonal change happening to your body, including changes in your weight, is completely normal.
Regardless of what you’re going through during menopause, you’re not the only one. Managing menopause symptoms like menopause weight gain is possible. Read on to better understand what’s going on with your hormones during menopause that might be causing weight changes and how to ensure you’re making your health a priority during this time.
Why Do Some People Gain Weight During Menopause?
During perimenopause, which can begin 8 to 10 years before menopause (usually your early to mid-40s), hormonal shifts leading up to menopause begin. The ovaries gradually stop producing as much estrogen—one of the main hormones that regulate your period—until eventually, they stop releasing eggs during the ovulation period each month. After 12 consecutive months without a period, you’ve reached menopause.
But these hormonal shifts aren’t exactly linear. “While progesterone follows a slow and steady decline, estrogen levels can rise and fall quite erratically, sometimes even the same day,” explains Sapna Shah, MD, an endocrinologist with Paloma Health.
So how does that play into menopause weight gain? Besides being a key player in your menstrual cycle, estrogen plays a role in storing fat on the thighs and hips, especially during your reproductive years, when you’d need more weight in those areas to sustain a healthy pregnancy.
When you get closer to menopause and estrogen levels drop off, that fat storage relocates to the abdominal area. More research needs to be done, but this seems to happen because estrogen is no longer circulating throughout the body and estrogen receptors change, redistributing more fat to the middle of the body.
It’s common to have wider hips, softer skin, and more weight, especially in the belly area. “But, you will not necessarily experience inevitable weight gain, especially if you are proactive in maintaining a healthy weight,” adds Dr. Shah.
Should You Be Concerned About Menopause Weight Gain?
Menopause isn’t the only reason you may gain weight as you get older. First of all, your metabolism slows as you age. You might also find yourself slightly less active and therefore burning fewer calories to begin with. The amount of body fat also increases as you get older. “It becomes easier for our bodies to store energy as fat instead of converting it into new muscle tissue,” explains Dr. Shah. “Not to mention, lipid turnover is reduced as we get older, so it is harder to shed fat with exercise.” Genetics play a role, too. So no, you shouldn’t have an immediate concern with a few extra pounds during menopause or post-menopause.
Just be mindful of the health risks associated with accumulating too much visceral fat (which is stored deep in the body, wrapping around the organs) in the belly area. “Deep belly fat is linked to an increased risk of type 2 diabetes, higher blood pressure, high cholesterol levels, and inflammation, all of which contribute to heart disease,” says Elizabeth Ward, MS, RDN, co-author of The Menopause Diet Plan: A Natural Guide to Hormones, Health, and Happiness.
Those cardiovascular risks associated with extreme weight gain can be dangerous because heart disease is the leading cause of death in postmenopausal women. Obesity is the real risk factor: It’s more prevalent after menopause, and affects 25 percent of postmenopausal women in the U.S., predisposing them to not only heart disease and diabetes but strokes, sleep apnea, and certain types of cancer.
Ultimately though, minor weight gain that you experience leading up to menopause or during the postmenopausal period is part of the natural hormonal process. Your weight won’t be the same as it was at age 25, nor does it need to be—your body doesn’t need to function in the same way as it did when you were 25. “Your optimal weight should be one where you feel your best and you are not increasing your risk for the health issues listed above,” Dr. Shah says.
How Can You Manage Menopause Weight Gain?
There are adjustments you can make to your diet and lifestyle to help mitigate some of the hormonal changes that can lead to menopause weight gain.
Go primarily plant-based.

There hasn’t been much research or instructions about specific diets to follow during menopause, Ward explains. One older study published by the American Heart Association found that pre-menopausal people between the ages of 44 and 50 who received nutritional guidance over a 5-year period about an eating plan had very little weight gain going into menopause. That eating plan focused on lowering their cholesterol and saturated fat intake as well as increasing their level of movement each week. (The Galveston Diet is also popular among people going through menopause, though no direct evidence has been done on it.)
What Ward recommends based on her own research is an eating plan that’s some combination of the Mediterranean style of eating and the DASH (Dietary Approaches to Stop Hypertension Diet, designed to keep blood pressure healthy. Go for at least 5 servings of fruits, vegetables, including legumes each day, plus 3 servings of whole grains and 3 servings of low-fat dairy foods (if you eat dairy), says Ward. She also recommends eating fish at least twice a week for heart-healthy omega-3s, and any other lean proteins you like.
This “diet” is less about adhering to or eliminating certain foods, and more about a whole foods-focused, balanced pattern of eating, which means limiting sugary and highly processed foods and alcohol as much as possible.
Prioritize Protein
“The most important nutritional change women going through perimenopause or menopause can do is increase dietary protein,” says Abby Grimm, MS, RDN, LD, a registered dietitian at FWDfuel Sports Nutrition. Protein intake, particularly from the amino acid leucine (found in both animal and plant-based sources of protein), is necessary to maintain and build more lean muscle, which in turn helps the body burn fat, Grimm says. Focusing on protein is not only key for lean muscle but for bone health as you age, adds Ward.
Minimize Simple Carbs
Because of changes in your metabolism, it may be more difficult to process carbohydrates. “As hormones are shifting, especially decreasing estrogen levels, the body is not able to build lean muscle as efficiently as it can with a normal menstrual cycle. This results in impaired utilization of carbohydrates and fat gain,” says Grimm.
You don’t need to eliminate carbs or follow a keto or Paleo-style diet, but shifting toward a more protein-heavy plan and decreasing your intake of simple, refined carbs is the objective, Ward says. Aim for fewer servings of sugary cereals, granola bars, bread and bagels, pastries, crackers, and chips, Grimm suggests.
Boost Mood and Muscle with Movement
Movement, especially resistance training of some kind (more on that below), coupled with eating more protein is going to help build that lean muscle as opposed to fat. But regular exercise nourishes your mental health too, particularly during the menopausal period, when anxiety and stress can spike. As Ward explains, elevated stress levels can impair weight loss and may contribute to weight gain due to the stress hormone, cortisol.
Grimm recommends an exercise routine that incorporates both strength training and some high-intensity interval training to get the heart rate up. “This type of exercise is much more effective than doing hours and hours of steady-state cardio when trying to limit visceral fat gain,” Grimm says. Those intense bursts of exercise that raise your heart rate way up can help the body burn fat and use glucose more efficiently.
Build Strength
When it comes to strength training, it’s worth picking up those dumbbells: A University of Arizona study found that a year of strength training helped postmenopausal women build more lean soft (aka fat-free) tissue in their bodies. Resistance training about three times a week also could reduce the symptoms of hot flashes, another trial found. The endorphins released during exercise could help the body regulate its own temperature, according to the research.
Lifting weights and HIIT workouts can both help the body reduce both inflammation and cortisol, Grimm adds.
Whatever You Do, Don’t Crash Diet
Restricting your eating by following strict “diets” or counting calories is not going to be sustainable for your weight or health during menopause, says Ward. Avoid cutting out food groups (unless you have a known allergy or intolerance), which can lead to inadequate nutrients needed to build muscle and reduce fat. “Fad diets may also be detrimental to your mental health if they cause you to be obsessed with food or otherwise trigger disordered eating,” Ward says. (Menopause can be a vulnerable time for your mental health in the first place.)
Get Your Sleep in Sync

26 percent of menopausal people have severe insomnia symptoms that disrupt their functioning the next day, reports Nature and Science of Sleep. One culprit might be that melatonin, one of the main hormones that regulate sleep in the body, dips during menopause.
The Takeaway on Menopause Weight Gain
Getting into the right sleep routine and getting enough sleep can help keep your metabolism on track and therefore help with healthy weight maintenance. “Having a specific bedtime and wake-up time can help regulate your circadian rhythm,” says Dr. Shah. Managing your stress and being able to wind down at night is a factor in this. Relaxing baths or showers in the evening rather than the morning can be part of a wind-down routine but also can lower the body’s core temperature and prepare the body to sleep, according to the Sleep Foundation. And especially during menopause, you’re going to want to sleep as cool as possible to avoid night sweats: so lower your bedroom thermostat, put cooling cotton or microfiber sheets on the bed, and sleep in super light pajamas or even moisture-wicking workout clothes to stay extra cool.
The post 7 Ways to Manage Menopause Weight Gain appeared first on HUM Nutrition Blog.
]]>The post How Hormones Impact Your Skin In Your 20s, 30s, 40s, And Beyond appeared first on HUM Nutrition Blog.
]]>The shift in sex hormones that occur as women age (and even throughout a single menstrual cycle!) can impact everything from sebum production, barrier function, collagen and hyaluronic acid production, and more.
The good news: Understanding how your short-term and long-term hormonal shifts influence your skin can help you target your skincare routine and lifestyle habits to support optimal skin health and appearance. Below, we cover the hormonal shifts you can expect to experience throughout your lifetime and simple, expert-approved strategies to help manage them.
The Key Players: How 3 Different Hormones Affect Skin

Before we dive into how hormones shift throughout a woman’s life—and what that means for skin health—it’s helpful to understand how specific sex hormones impact your skin. As with most other cells in your body, various types of cells within your skin have receptors for different hormones, and the presence or absence of these hormones can lead to different skin manifestations.
While non-sex hormones such as cortisol (a stress hormone) can impact the skin, to an extent, we’ll hone in on the ones that make the biggest difference: estrogen, progesterone, and androgens.
Estrogen
“Estrogen is key for the normal functioning of the skin as well as the blood vessels, hair follicles, oil glands, and our pigment-producing cells called melanocytes,” says Keira Barr, MD, a dual board-certified dermatologist and menopause specialist and author of The Skin Whisperer. “It is associated with collagen production, increased skin thickness, increased hyaluronic acid production, improved skin barrier function, maintaining skin hydration, reduced sebaceous (oil) gland activity, and improved wound healing. It also plays a role in modulating inflammation.”
Progesterone
The effect of progesterone on the skin is less well defined, but, according to Dr. Barr, it’s thought to contribute to skin elasticity, pigmentation, and the increased circulation and sebaceous gland activity that is observed in the second half of the menstrual cycle.
Androgens
Androgens, which are normally thought of as male hormones, can also impact women’s skin. These hormones, including testosterone, are produced in small amounts by the female body and play a role in oil gland production. When hormones are imbalanced—as can occur in women with PCOS and when women experience comparatively elevated androgen levels during menopause—androgens may also contribute to unwanted facial hair growth.
In your 20s and 30s
A lot can be going on in your 20s and 30s. Acne, which is often associated with adolescence, can still affect many women during this time period, and it can have a lot to do with the hormonal shifts that occur during womens’ monthly cycles. In fact, research shows that about 50 percent of women in their 20s and 35 percent of women in their 30s experience acne.
But in addition to periodic bouts of acne, skin can also vary in its moisture content, sensitivity, and general radiance depending on the time of the month. Here, we break down the typical hormonal changes that occur throughout a menstruating woman’s cycle, how they affect skin, and what you can do about it:
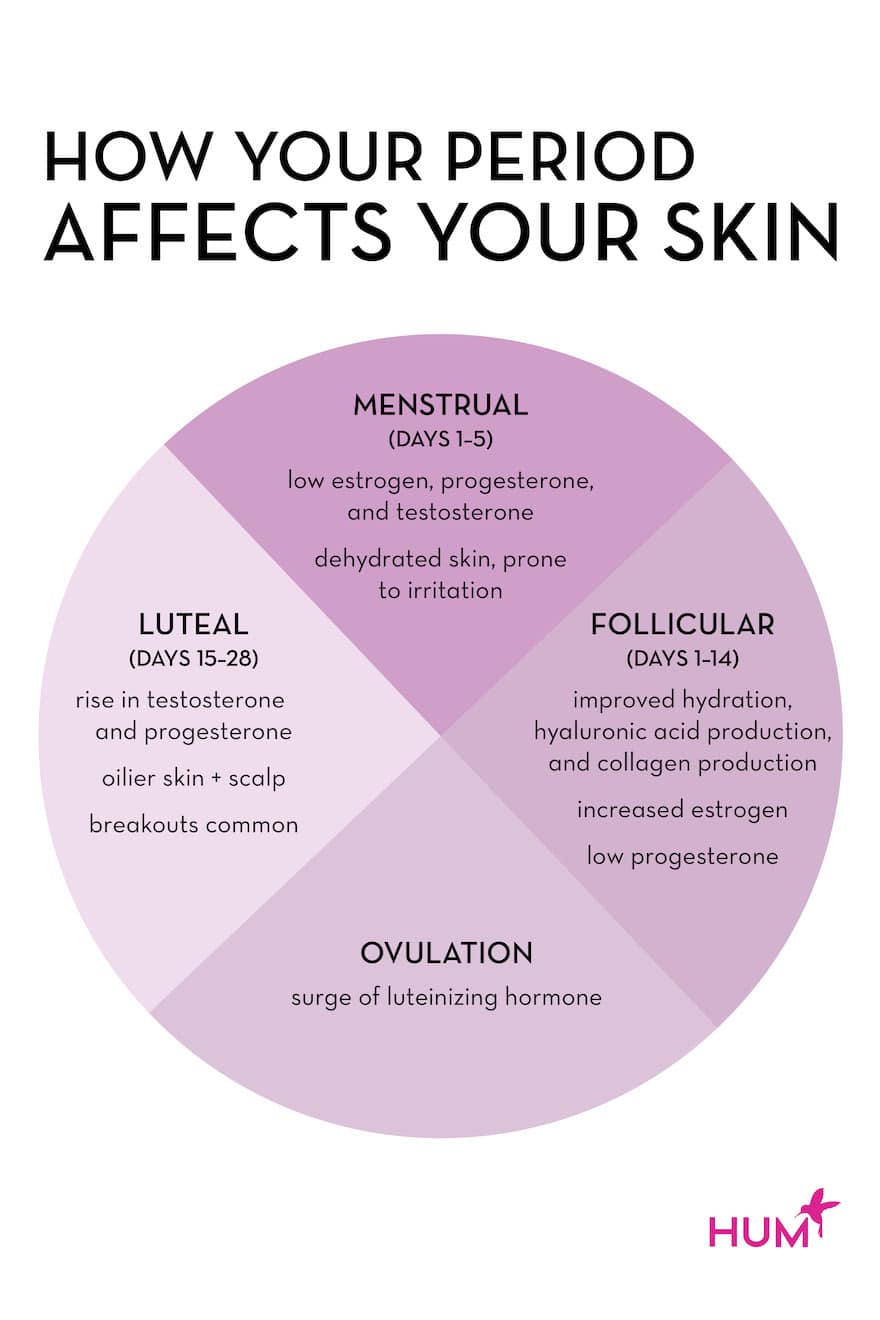
Menstruation (days 1-5)
Each menstrual cycle starts with menstruation, or your period. This takes place in the very beginning of the follicular phase. “During this phase, levels of estrogen are at their lowest, which translates to a decrease in skin hydration and vulnerability of the skin barrier to irritation and inflammation,” says Dr. Barr. “With both progesterone and testosterone also low, there is less sebaceous gland activity and oil production, contributing to skin dryness.”
Cumulatively, this can all add up to dehydrated skin that’s more prone to irritation and inflammation. According to Dr. Barr, this is why conditions like atopic dermatitis (eczema), contact dermatitis, and psoriasis, may be worse just before or during your period.
What you can do: Moisturizing with soothing and nourishing skincare ingredients is often your best bet. Opt for gentle cleansers and look for things like hyaluronic acid, ceramides, gotu kola, and sea buckthorn oil on ingredient lists, suggests Dr. Barr. Scaling back on abrasive exfoliants and products containing too many active ingredients, including topical retinoids and chemical exfoliants, may also help if you’re prone to irritation. Finally, drinking plenty of water and eating foods rich in omega-3 fats, vitamin C, and antioxidants can help ease inflammation and irritation, support a healthy skin barrier, and promote hydration from the inside out.
Follicular phase (days 1-14)
After your period, the remainder of your follicular phase is characterized by increases in estrogen levels, which peak around day 14 (when most women ovulate). “This translates to a boost in skin barrier function, skin hydration, hyaluronic acid production, and collagen production,” says Dr. Barr. “Skin is typically smoother, calmer, and more radiant than other times of the month, as estrogen peaks at ovulation and progesterone is still low, which means those sebaceous glands are pumping out less oil.”
What you can do: You don’t need to do much at all! This is a time to embrace your natural glow and take a break from makeup—but don’t forget your moisturizer with SPF—due to estrogen’s effect on pigment-producing cells, you want to be sure to protect your skin from UV rays, warns Dr. Barr. Using products with more active ingredients such as alpha-hydroxy acids (e.g. glycolic acid, lactic acid) and retinoids is usually better tolerated during this time of the month since skin barrier function is optimal.
Luteal Phase (days 15-28)
Here’s when things can get a little…greasy. When you ovulate on day 14, there is a surge in luteinizing hormone (LH), which prompts a rise in progesterone and testosterone, and “these two hormones contribute to increased sebaceous gland activity and oilier skin, including an oily scalp,” says Dr. Barr. “Additionally, estrogen levels are low relative to progesterone, so there may be more inflammation, irritation, and disruption of the skin barrier, which may contribute to breakouts.”
In fact, 60-70 percent of women experience these mild premenstrual flares of acne. The lower half of the cheeks, the chin, and the jawline region are the most common areas for these hormonal acne breakouts, says Zenovia Gabriel, MD, FAAD, who specializes in hormonal dermatology.
Towards the end of the luteal phase, estrogen continues to decline and progesterone decreases as well, transitioning your skin to that dryer, more dehydrated, inflamed state that can be typical during menstruation, as previously discussed.
What you can do: If you notice that your skin is more oily and prone to acne, adding a toner after cleansing may be helpful. Look for ingredients like salicylic acid, benzoyl peroxide, tea tree oil, and witch hazel, which may help kill the bacteria associated with acne and accelerate cellular turnover. But don’t go overboard with products that strip the skin of oil, cautions Dr. Barr, as this could actually cause your skin to oversecrete oil.
Acne is also a very inflammatory condition, so nourishing your body with anti-inflammatory foods rich in omega-3 fats, vitamin C, and antioxidants may be beneficial, as well as scaling back on added sugars and dairy, since these have both been linked to hormonal breakouts. Getting good sleep, exercising, meditating, and connecting with friends and family are all activities that can help curb inflammation as well, says Dr. Barr.
Other factors in your 20s and 30s

In addition to these “typical” hormonal shifts that most women in their 20s and 30s experience, other factors can affect hormones and thus skin health—namely, birth control pills and stress.
Hormonal birth control comes in many forms, but often, doctors prescribe combined oral hormonal contraceptives—pills that contain synthetic forms of both estrogen and progesterone, especially for women struggling with acne, menstrual cramps, or irregular periods. The data shows that combined contraceptives, as a class, exhibit a pro-estrogen effect on the skin and reduce the production of androgens, making them helpful for these issues, says Dr. Zenovia. However, it’s important to note that once someone stops taking birth control, these issues will often reemerge as they don’t get to the root of any potential hormonal imbalances.
Your 20s and 30s are often packed with particularly stressful transition periods as well (think: entering the workforce, navigating new relationships, having babies, etc). Research has shown that psychological stress can negatively impact skin barrier function, which, in turn, may trigger or exacerbate eczema, psoriasis, acne, and overall skin irritation. This may be due to elevated levels of the stress hormone cortisol, which is associated with inflammation and inflammatory skin conditions. So, anything you can do to curb the effects of stress—exercising, meditating, talking to a therapist—may help your skin, too.
Pregnancy

During pregnancy, increased levels of estrogen and progesterone lead to increases in melanin stimulating hormone (MSH), which stimulates pigment cells called melanocytes. This, in turn, can contribute to darker moles, darker nipples, a darker vulva, and even melasma says Dr. Zenovia. Melasma during pregnancy is called chloasma. It affects about 45–75 percent of pregnant women and is characterized by patchy brown spots often occurring on the forehead, upper lip, and cheeks due to increased production of melanin by melanocytes.
For some women, pregnancy may also increase sebum production, which may or may not lead to acne. During pregnancy, the body also increases blood production by about 50 percent, which may boost circulation and contribute to an overall brighter complexion. Together, these factors may contribute to that dewy, rosy so-called pregnancy glow.
What you can do: Pregnancy-induced melasma is directly stimulated and worsened by UV exposure, so it’s crucial to reduce your sun exposure, wear protective clothing, or use a physical (a.k.a. mineral-based) sunscreen, says Dr. Zenovia. If your melasma is minor, it will typically resolve postpartum. If you happen to experience acne, your options are a bit limited during pregnancy, but The American College of Obstetricians and Gynecologists says it’s safe to use topical glycolic acid, azelaic acid, benzoyl peroxide, and salicylic acid.
In your 40s and 50s
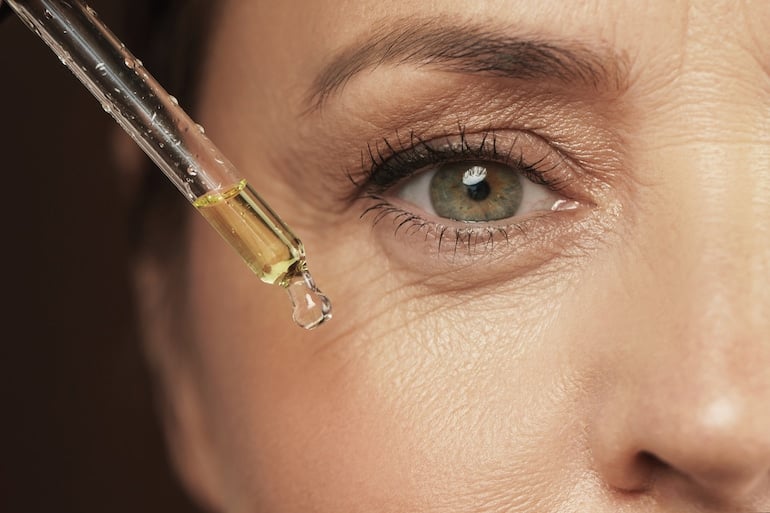
Depending on your health and your hormones, your 40s might look a lot like your 30s. If you’re menstruating regularly, many of the cyclical hormonal fluctuations and recommendations above will still apply to you. Likewise, if you’re pregnant in your 40s, check out the tips above.
However, for many women, their 40s are characterized by irregular periods and fluctuations in estrogen and progesterone levels that eventually lead to significant drops in these hormones. This transition period is called perimenopause, and once you’ve gone through 12 consecutive months without a period, you’ve officially reached menopause. Most women hit menopause between age 45 and 50, with an average age of 51.
“When our hormones [estrogen and progesterone] diminish during perimenopause and postmenopause, the functions they perform to maintain the health and vitality of the skin diminish as well,” says Dr. Barr.
The skin is full of estrogen receptors, and when estrogen binds to those receptors, it stimulates the production of hyaluronic acid, which enhances hydration and plumps skin, as well as the synthesis of collagen and elastin, which contribute to skin’s firmness and resiliency. “But without estrogen’s influence, pores will appear larger and fine lines, wrinkles, and sagging skin becomes more prominent,” says Dr. Barr. In fact, research suggests that women lose around 30 percent of their collagen in the five years following menopause, so the changes can be quite significant.
But that’s not all. There’s also a decline in sebum production and circulation that can alter the skin’s barrier, resulting in skin that’s dry, sensitive, and prone to irritation and inflammation, according to Dr. Barr. Skin cellular turnover (how quickly skin cells can replace themselves) also declines, which not only gives skin a generally dull appearance but contributes to slower wound healing and age spots. Skin also has a reduced ability to handle oxidative damage from sun exposure, which can increase skin cancer risk.
What you can do: While there’s a lot that’s seemingly going wrong with your skin during this time, there’s also a lot you can do! First and foremost, due to your skin’s reduced ability to handle oxidative stress, using sunscreen daily is a must.
To battle dryness, you’ll also want to use gentle, non-foaming cleansers and products with soothing and nourishing skincare ingredients, including hyaluronic acid, ceramides, gotu kola, and sea buckthorn oil, suggests Dr. Barr. Drinking plenty of water and eating foods rich in omega-3 fats, vitamin C, and antioxidants can also help ease inflammation and promote hydration. Some research even suggests that oral collagen supplements can improve skin’s moisture levels and elasticity.
To support skin cell turnover and enhance collagen production, consider trying a topical retinol product, suggests Dr. Zenovia. Retinol increases the turnover rate of keratinocytes, which helps skin appear smoother and dewier, and helps unclog pores. Over time, research shows it can support collagen production in the dermis and inhibit the breakdown of collagen. However, retinol can be irritating for some people and it increases your skin’s sensitivity to the sun. For something gentler, consider a serum or cream containing the plant-derived ingredient bakuchiol, which supports skin cell turnover without increasing photosensitivity.
The Takeaway

Your skin and hormones are connected, so as your hormone levels change throughout your life, knowing how those changes affect your skin can help you look and feel your best. Don’t be intimidated by these different stages—there are plenty of products and lifestyle changes that can help your skin thrive.
The post How Hormones Impact Your Skin In Your 20s, 30s, 40s, And Beyond appeared first on HUM Nutrition Blog.
]]>The post This Menopause Supplement Will Help You Cool Down and Feel More You Again appeared first on HUM Nutrition Blog.
]]>Jennifer Martin-Biggers, PhD, MS, RDN, HUM’s VP of scientific affairs and education explains why supplements for menopause can make this time easier and how Fan Club’s star ingredients help to reduce 11 common symptoms of menopause and perimenopause, so you can get back to conquering the world (or, you know, your to-do list.)
A Menopause Supplement that Actually Works
Every person with a uterus will go through menopause—that’s half of the world’s population. Still, most women aren’t even sure exactly what perimenopause and menopause are and what they should expect until they’re experiencing it for themselves. 60 percent of women say the physical and mental effects of declining hormone levels aren’t discussed enough, leaving them feeling unprepared for menopause. Not only that but there are so few products available to help women cope with symptoms.
“Menopause is still a taboo subject that is not commonly discussed, yet we heard from our customers over and over that they wanted something to help manage their menopause symptoms,” explains Dr. Martin-Biggers.
In fact, 7 in 10 women have not received any treatment for their symptoms.
At HUM, we want to change this so women going through perimenopause or who are post-menopausal can be more confident, energized, and feel themselves again. No one should have to go through menopause alone.
Just think of us as your biggest fans, cheering you on along the way. That’s where Fan Club comes in.
What is Fan Club?
“Fan Club is a non-hormonal, clinically studied dietary supplement that plays the role of your biggest fan, helping to smooth out the decline of estrogen that can cause menopause symptoms,” says Dr. Martin-Biggers.
“For medical or personal reasons, some women may not be able to take hormonal treatments prescribed by a doctor, like hormone replacement therapy, or other supplements that directly affect estrogen levels,” explains Dr. Martin-Biggers. “Fan Club is an estrogen-free supplement that does not affect hormone levels and has been studied to be safe with prolonged use. It’s a great supplement for someone looking for a non-hormonal option.”

Fan Club features three ingredients: Siberian rhubarb root extract, Lactobacillus Plantarum DR7, and grape seed extract.
Overall benefits that the trio have provided in clinical studies include:
- 83% reduction in total menopausal discomforts
- 83% reduction in hot flashes
- 66% reduction in irritability and mood swings
- Optimized gut microflora balance
More on these benefits and ingredients soon.
What Causes Menopause Symptoms, Anyway?
Every person going through menopause will experience it differently, but most menopause symptoms all tie back to a gradual decline in the hormone estrogen. Estrogen typically begins to drop in your 40s, and this can cause a ripple effect on other hormones and processes throughout the body, leading to a range of symptoms.
The most common sign of perimenopause, of course, is getting menstrual periods less often and changes to length and flow. But other symptoms are also common in the 4-8 years leading up to menopause. Some women may even experience symptoms post-menopause, or after it’s been one full year without a period.
11 Common Symptoms of Menopause
- Hot flashes + night sweats
- Vaginal dryness
- Fatigue
- Mood swings
- Irritability
- Restlessness
- Sleeplessness
- Heart racing
- Low sex drive
- Bladder problems
- Joint and muscle discomfort
The Top Ingredients to Help Reduce Menopause Symptoms
To reduce the many symptoms that women experience during menopause, we looked at the most clinically effective ingredients and doses of ingredients and identified three standouts.

Siberian Rhubarb Root Extract
We sourced ErR731Ⓡ, a special extract of Siberian rhubarb root, to combat the most disruptive menopause symptoms. “It has undergone rigorous clinical testing and consistently shown beneficial effects and safety in every study,” says Dr. Martin-Biggers. This extract reduced hot flashes by 83 percent and decreased the severity, found a 2006 clinical study in the journal Menopause. Siberian rhubarb root extract has also been shown to improve night sweats, heart racing, sleep disturbances, mood swings, irritability, restlessness, fatigue, sex drive, vaginal dryness, and joint and muscle discomfort associated with menopause.
Scientists believe molecules from the extract stimulate an estrogen receptor, tricking your body into thinking it’s estrogen and evening out the symptoms associated with estrogen’s unstable decline.
Lactobacillus Plantarum DR7
Probiotics for menopause!? Yes! This super-strain reduced symptoms of stress, improved mood, and reduced levels of the stress hormone cortisol in clinical studies.
Your brain and gut are connected via the gut-brain axis, so positive changes in your gut health can boost mood.
This probiotic has also been studied to evaluate its effects directly on mood. A 2020 study discovered Lactobacillus plantarum DR7 helps to increase serotonin and other chemicals that support brain health and mood.
Grape Seed Extract
Not your average grape, we packed Fan Club with a proprietary extract of grape seed. Studies show it helps relax and control blood vessels, improving symptoms like hot flashes and sweating and reduces perceived stress and worry.
A study of 96 women with at least one menopausal symptom significantly improved their symptom scores at 8 weeks and mood scores after just 4 weeks.
Grape seed extract contains a concentrated amount of the powerful antioxidant proanthocyanidin, which can increase your body’s natural production of nitric oxide. Nitric oxide is needed to help oxygen, blood, and nutrients travel throughout your body.
Join Our Fan Club
“We recommend taking Fan Club in the morning with food, so you don’t forget later in the day,” says Dr. Martin-Biggers. “Results may be seen after 1 month, but it takes around 2 months for the results to fully be seen.” The best part about Fan Club is that because of its safety, you can take it as long as you need relief from menopause symptoms.
Your HUM Line-up for Menopause Support

New to HUM or looking for more ways to support your body during the perimenopause or post-menopausal phase?
These supplements pair well with Fan Club:
- Mighty Night
Many women going through menopause experience sleep issues due to (you guessed it!) the decline in estrogen. The valerian root, passion flower, and hops in Mighty Night help promote deeper sleep, plus you get the added bonus of ceramides, ferulic acid, and CoQ10 to promote healthy-looking skin.
- Collagen Love
Collagen, which keeps skin looking firm and plump, declines by about 1 percent each year, starting in your 20s. Collagen Love features collagen peptides to support skin firmness and elasticity.
- Here Comes The Sun
It can be hard to get enough vitamin D from sunlight and the need for vitamin D increase as you mature. Here Comes The Sun delivers 250 percent of your recommended daily vitamin D intake.
Ready to wave hot flashes goodbye? Check out Fan Club for yourself and be sure to reach out to your personal HUM RD to get the scoop on how you can use nutrition to support perimenopause and menopause.
The post This Menopause Supplement Will Help You Cool Down and Feel More You Again appeared first on HUM Nutrition Blog.
]]>












